In March 2017, a mini-symposium at the 11th Congress of Controversies in Neurology (CONy), Athens, Greece, was dedicated to neuro-Behçet’s disease (NBD). An introduction into the key clinical features of Behçet’s disease (BD) was followed by a review of its neurological manifestations and a focused presentation of the challenges of differential diagnosis. This review represents a report of the mini-symposium in the form of an updated summary of the topics that were presented. It follows the structure of the mini-symposium and in part expands the information presented there. However, a systematic review is beyond the scope of this report. The general introduction to BD will be succinct, as the focus of this review is NBD. Details of BD in general can be found in recent reviews, for example, Yazici et al.1
Behçet’s disease
History and epidemiology
BD is a chronic, multisystemic and polysymptomatic disease with unpredictable exacerbations and remissions. All systems can be affected concomitantly or consecutively.1 There are several clinical subsets and there is geographical variation indicating different disease mechanisms. In view of this, some authors favour using the term Behçet’s syndrome rather than Behçet’s disease. For consistency and harmonisation purposes, and to follow the terminology of the discussions of the mini-symposium, this review will use the term Behçet’s disease. In 1930, the ophthalmologist Adamantiades described the coexistence of ocular, skin and mucous lesions in one patient.2 In 1937, Hulusi Behçet identified BD in two patients, who were suffering from oral and genital ulcers, in addition to eye disease and described it as a separate disease believed to be caused by a virus.3
Epidemiologic studies have shown a wide variability in the prevalence of BD depending on the geographic and ethnic origins of the population. Evidence shows that the prevalence of BD is higher in the areas in which the population has a high incidence of HLA-B51 allele.4 It is often called ‘silk road disease’ because of its relatively high prevalence in Mediterranean, Middle Eastern and Far Eastern countries across the ancient silk trading route. Turkey has the highest prevalence, at 119.8 per 100,000.4
Pathophysiology
The pathomechanisms of BD are not fully known; however, it can be viewed as a condition associated with autoimmune responses, autoinflammation and vascular injury. Susceptibility seems to be determined by an interplay between genetic and environmental factors. Among the susceptibility genes, those for cytokines such as interleukin (IL)-17, IL-12, IL-23, IL-21, IL-23, tumour necrosis factor (TNF)-α, IL-1β and IL-8 have been implicated.5 Dysregulation of these pro-inflammatory cytokines may reflect an uncontrolled activation of the innate immune system with or without activation of the adaptive immune responses that appear to be responsible for the pathological features. Elevated production of pro-inflammatory cytokines, such as TNF-α, IL-1β and IL-8, results in the activation of neutrophils and the augmentation of cellular interactions between neutrophils and endothelial cells.6 These activated neutrophils produce excessive superoxides and lysosomal enzymes which bring about tissue injury. The resulting lesions are characterised histologically by neutrophilic angiocentric infiltrates with leukocytoclastic (early) or lymphocytic (late) vasculitis with or without mural thrombosis and necrosis.7 In addition, B lymphocyte function has been reported to be abnormal in some patients.8
Among the environmental factors responsible for susceptibility to BD, infectious agents that have been implicated most frequently include bacteria such as Streptococcus sanguinisand viruses, mainly herpesviruses. Indeed, the gene–environment interaction in BD is indicated by dense genotyping studies linking dysregulated host immune response to bacterial antigens to the BD susceptibility.9
Clinical manifestations and diagnosis
BD has a wide range of clinical manifestations. Oral ulcers are usually the first symptom; they may appear years before the diagnosis and are present during the disease course at almost 100% frequency. In 75% of patients, anogenital aphthae are seen, primarily on the scrotum and penis in men and the vulva in women. In around 60% of patients, various cutaneous lesions have been reported, which include erythema nodosum, papullopustular lesions, pseudofolliculitis, pyoderma gangrenosum, and cutaneous vasculitis.1,10
In addition, numerous other areas are commonly affected by BD. Ocular presentations of BD occur in 30–80% of patients (predominantly in men) and are a major cause of morbidity as they can result in blindness, particularly in the setting of retinal vasculitis.1 Joint involvement is also commonly reported in BD. Mono/polyarthritis in BD is Italicsnon-erosive and the most affected joints are knees, ankles, feet and Italicshands. Gastrointestinal involvement is characterised by pain, haemorrhage, gut mucosal ulcerations or intestinal perforation. ItalicsVascular involvement may also occur, most commonly deep/superficial peripheral venous thrombosis and also aneurysmal/occlusive arterial disease. Cardiac involvement includes coronary arteritis, vascular disease, intracardiac thrombi or thrombosis of venous collateral vessels and superior vena cava, myocarditis and recurrent ventricular arrhythmias.1 Neurological involvement is also a common manifestation of BD, and will be discussed further in the following section.
The diagnostic criteria for BD were published 28 years ago.11 The major criterion is recurring oral ulcerations (aphthous or herpetiform) observed by the physician or reliably reported by the patient at least three times in a 12-month period. In addition, two of the four minor criteria must be fulfilled:
- recurrent genital ulceration;
- eye lesions: anterior uveitis, posterior uveitis, cells in the vitreous by slit lamp examination or retinal vasculitis observed by an ophthalmologist;
- skin lesions: erythema nodosum, pseudofolliculitis, papulopustular lesions or acneiform nodules in post-adolescent patients not on corticosteroids; and
- a positive pathergy test (skin prick test): non-specific skin Italicshyper-reactivity in response to minor trauma read by a physician at 24–48 hours (>2 mm pustule, after forearm skin (5 mm depth) prick with 20–22 g needle).
Treatment options
The goal of BD treatment is to promptly suppress inflammatory exacerbations and recurrences to prevent irreversible organ damage and a multidisciplinary approach is necessary. The management of BD depends on whether there are self-limiting manifestations or serious organ involvement, and should be individualised according to age, gender and type.12,13 In systemic severe disease, intravenous pulse corticosteroids followed by daily oral doses, azathioprine, cyclophosphamide, cyclosporine-A, methotrexate, mycophenolate mofetil, tacrolimus, interferon (IFN)-α or TNF-α inhibitors (etanercept, infliximab) can be chosen.12 A new oral inhibitor of phosphodiesterase-4, apremilast, has been studied in patients without major organ involvement and demonstrated a complete response in significantly more patients.14
Other treatments aim to control the specific symptoms of BD. TNF-α inhibitors are highly effective in BD, particularly in ocular involvement.15,16,17 Long-term administration of the TNF-α inhibitor infliximab may reduce the frequency of ocular recurrences, even in resistant cases. As a first-line treatment, infliximab should be started in conjunction with an immunosuppressive drug (azathioprine, corticosteroids or Italicsmethotrexate) and upon occurrence of remission, concomitant corticosteroids should be reduced. Many studies have demonstrated the effectiveness of infliximab in BD.15–17 In patients with posterior segment eye involvement, azathioprine, cyclosporine-A, IFN-α or anti-TNF-α often combined with systemic corticosteroids, should be initiated. In patients with posterior segment eye involvement, azathioprine, cyclosporine-A, IFN-α or anti-TNF-α often combined with systemic corticosteroids, should be initiated.12,13
For the management of major vessel disease with thrombotic events in BD, corticosteroids and immunosuppressants such as azathioprine, cyclophosphamide or cyclosporine-A are recommended,12 and Italicsanti-TNF-α could be considered in refractory patients. Anticoagulants are considered when the risk of bleeding, in general, is low and coexistent pulmonary artery aneurysms are ruled out.12,13 For gastrointestinal symptoms, 5-aminosalicylic acid derivatives, including sulfasalazine or mesalamine, systemic corticosteroids, azathioprine, anti-TNF-α, and thalidomide may be used. Central nervous system involvement, including acute attacks of cerebral parenchymal involvement, are treated with high-dose corticosteroids followed by tapering, together with immunosuppressants. Cyclosporine, although inexpensive, should be avoided due to the risk of neurotoxicity. Anti-TNF-α should be considered in severe or refractory disease as Italicsfirst-line. The first episode of cerebral vein thrombosis (CVT) should be treated with high-dose corticosteroids, followed by tapering. Anticoagulants may be added for a short duration.
Neurological involvement in Behçet’s disease
As with systemic disease, the neurological manifestations of BD are varied.18–22 Neurological involvement in BD can be classified as; 1) primary, in which the neurological involvement is directly due to BD and is named as NBD or neuro-Behçet’s syndrome (NBS); and 2) secondary, in which the neurological manifestations are the result of neurologic complications secondary to systemic involvement of BD (i.e. cerebral emboli from cardiac complications of BD, increased intracranial pressure secondary to superior vena cava syndrome) or due to the therapies used for the systemic manifestations of BD (i.e. central nervous system [CNS] neurotoxicity with cyclosporine; peripheral neuropathy secondary to thalidomide or colchicine). These are indirect causes of neurological problems in patients with BD and are not termed as NBD.
Primary neurological involvement with NBD occurs in up to 10% of all patients.18–22 NBD normally presents within the fourth decade and approximately 5 years after the onset of the systemic disease. Although some patients may present with neurological involvement without fulfilling the International Study Group (ISG) classification criteria for BD,11 and a diagnosis of NBD cannot typically be made unless there are at least the history or sequelae of some of the systemic manifestations of BD. Although BD is seen almost equally in both genders, NBD is more common in males (3:1).23 BD and NBD are rare in the paediatric population; however, when neurologic involvement occurs in children it is often soon after the onset of the systemic disease.20.21
Clinical and neuroimaging findings indicate that there are two major forms of NBD: 1) CNS inflammatory parenchymal disease (p-NBD); and, less commonly, 2) an extra-parenchymal form (ep-NBD) that involves large extra-parenchymal vascular structures, mainly venous dural sinuses, causing cerebral venous sinus thrombosis (CVST). In contrast to p-NBD, CVST is more commonly observed in paediatric patients with NBD and these two types of involvement occur very rarely in the same individual and, thus, are likely to have different pathogeneses. Rarely, an aseptic meningitis may be the presentation of extra-parenchymal NBD. Behavioural and psychotic symptoms, which are termed as ‘neuro-psycho-Behçet’, may be observed during the course of NBD. Cognitive functions are also likely to be affected in a subgroup of patients with BD and frontal (executive) dysfunction is the most common pattern observed. Primary peripheral nervous system involvement has been reported in BD, but is extremely rare.18,19
The most common neurological symptom seen in NBD is headache, which occurs both in parenchymal (p-NBD) and extra-parenchymal NBD (ep-NBD, CVST). However, headache may also be a symptom of severe ocular inflammation; may be associated with exacerbations of systemic symptoms of BD, with some migraine-like features, and is referred to as the ‘nonstructural headache of BD’; or may be independent of BD and may coexist as a primary headache at similar rates with the general population. Other common symptoms are weakness (hemiparesis), gait disturbances (ataxia), speech difficulties (dysarthria) and less commonly, behavioural and cognitive changes. Visual loss due to optic neuritis, sensory and extrapyramidal symptoms and seizures are rare.18–22
The International Consensus Recommendation (ICR) criteria are suggested to be used in diagnosing NBD.24 These criteria can be summarised as ‘the occurrence of neurological symptoms and signs in a patient who meets the ISG Diagnostic Criteria for BD that are not otherwise explained by any other known systemic or neurological disease or treatment and in whom objective abnormalities consistent with NBD are detected either on neurological examination, neuroimaging studies, MRI, or abnormal cerebrospinal fluid (CSF) examinations’.24 The ICR criteria also include a ‘probable NBD’ criteria, but one should be more prudent in making such a diagnosis.
Parenchymal neuro-Behçet’s disease
About 75–80% of patients with NBD present with parenchymal involvement. The major symptoms and signs of p-NBS include headache, dysarthria, ataxia, hemiparesis and cranial neuropathies (mainly involvement of motor-ocular and facial nerves) and these usually develop in a subacute manner. p-NBD is one of the major causes of morbidity and mortality in NBD. Similar to multiple sclerosis (MS), the clinical course of p-NBD may remain with a single attack, may have a relapsing form, or may be progressive. However, patients with p-NBD usually are left with neurologic deficits. The lesions of p-NBD lesions commonly involve the telencephalic/diencephalic junction and the brainstem, which are usually large, with no distinct borders. In the acute phase these lesions are likely to enhance and generally appear in a heterogeneous pattern. Tumefactive cerebral lesions may be seen, and spinal cord lesions, although not common, when occurring are likely to be longitudinally extensive. In these patients, anti-MOG and AQP4 antibodies are typically absent. Cerebellar focal involvement is uncommon, but isolated cerebellar atrophy has been reported.25 Lesions in intra-parenchymal major arterial territories are unusual and involvement of large extra-parenchymal or smaller intra-parenchymal arteries although extremely rare have been reported, suggesting that a subgroup of arterial p-NBD may exist.26 Based on the radiological and histopathological findings, a venous pathogenesis is the likely explanation of p-NBS lesions.17–19,26
The CSF findings may disclose a prominent pleocytosis and an elevated protein level during the acute episode of p-NBD. Neutrophilic predominance is typical during the acute phase, but this later is replaced by a lymphocytic form. Oligoclonal bands are rarely detected.
Extra-parenchymal neuro-Behçet’s disease/cerebral venous sinus thrombosis
Up to 20% of patients with NBD have CVST. These patients present with severe headache, which usually develops over a few weeks. Typically, the funduscopic and neurological examination shows papilledema and occasionally a sixth nerve palsy. Compared with other causes of dural sinus thrombosis, impaired consciousness, focal neurologic deficits such as hemiparesis and epileptic seizures are uncommon in extra-parenchymal NBD, and venous infarcts are unlikely. A magnetic resonance venography will confirm the diagnosis and show the extent of CVST. With the exception of an elevated opening pressure, the CSF findings are generally normal, except in the rare meningitic presentation where a high number of neutrophils can be found. As already mentioned this form of NBD occurs more commonly in the paediatric population suggesting that age may influence the form of neurological involvement.
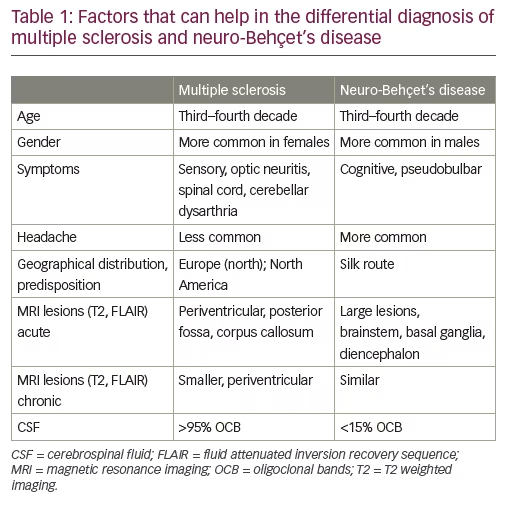
Neuro-Behçet’s disease – differential diagnosis
The differential diagnosis of NBD remains a major challenge. Particularly difficult are situations in which a patient without full blown BD presents with neurological manifestations. It is important to know that neurological manifestations of BD reflect more severe disease, and are rarely seen in isolation. Therefore, clinicians suspecting NBD must be vigilant to look for the likely development of symptoms and signs outside the CNS. This is also important in patients with known BD, as neurological manifestations tend to appear during severe flare-ups, and systemic BD manifestations should be sought. In meningitic presentations, the differential diagnosis from acute bacterial meningitis is essential. Acute bacterial meningitis is a medical emergency and antibiotic treatment is often initiated in emergency settings before the microbiological confirmation. Although the CSF in meningitic NBD often has fewer leucocytes, it can sometimes reach the numbers encountered in bacterial meningitis and failure of recognition may have serious consequences. A transient clinical improvement can be seen following institution of supportive measures and antibiotics, which may delay the aggressive treatment of BD.
Uveomeningeal syndromes are a heterogeneous group of inflammatory disorders characterised by meningeal inflammation and eye involvement (uveitis).27 The differential diagnosis includes many entities, and associated systemic features, specific organ involvement (e.g. lung in sarcoidosis) and imaging and biomarker characteristics can help distinguish NBD from the other conditions. In addition to NBD, uveomeningeal syndromes include:
- sarcoidosis;
- granulomatosis with polyangiitis;
- syphilis;
- Vogt-Koyanagi-Harada disease; and
- acute posterior multifocal placoid pigment epitheliopathy.
One of the most important and challenging considerations in the differential diagnosis of NBD is MS.18,28 When the diagnosis for either entity is well established, distinction is relatively easy; however, in the initial phases, the distinction can be difficult. The parenchymal lesions of NBD can mimic those of MS on MRI in most aspects, including the ovoid shape of callosal ‘Dawson’s fingers’ and the presence of a central vein. Due to the perivenular distribution of lesions in both conditions, the utility of the central sign and its role in the differential diagnosis of MS versus NBD remains subject to debate in expert consensus discussions.28,29 While this is particularly relevant early in the disease and recent evidence shows that more MS than NBD white matter lesions have central veins, one needs to bear in mind that generally, patients with NBD have fewer white matter lesions than patients with MS, so using the central vein for distinction may remain difficult. Other issues that have been helpful in distinguishing the two entities can be seen in Table 1. It is important to note that the initial manifestation of NBD can be a tumefactive brain lesion, which can be almost indistinguishable from both a tumefactive MS presentation and a brain tumour, the latter being an essential differential diagnosis consideration.30,31 Clinicians need to be aware that NBD and MS need not be mutually exclusive. Indeed, a group of patients with established NBD also fulfil the diagnostic criteria for MS and have clinical, imaging and laboratory features (oligoclonal bands in the CSF) of MS.32
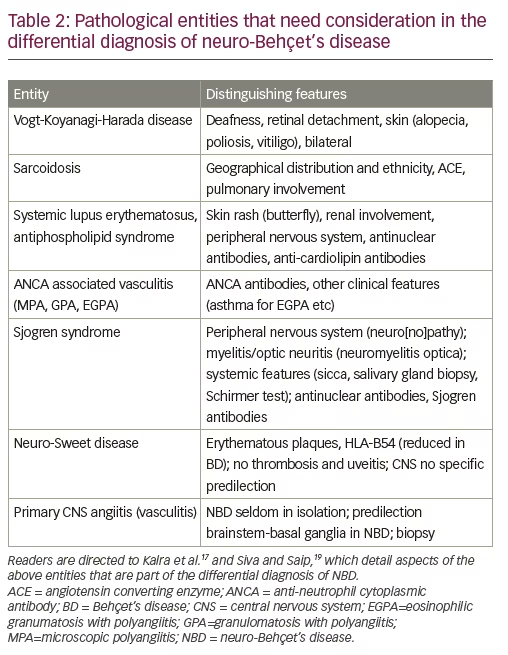
Another important aspect of the differential diagnosis is systemic vasculitis, which can be primary or secondary to other systemic inflammatory diseases with neurological manifestations. Table 2 presents a list of systemic inflammatory disease with or without secondary vasculitis which can be misdiagnosed as NBD and their distinguishing features which can help in the differential diagnostic of NBD. These are discussed in more detail in Kalra et al. and Siva and Saip.18,24
In patients presenting with acute stroke, the vascular variant of NBD sometimes represents part of the differential diagnosis. To distinguish from non-vasculitis atherosclerotic stroke, it is helpful to bear in mind the higher frequency of venous thrombosis compared to arterial territory stroke in NBD. On the other hand, some strokes in NBD involve arterial territories, so an arterial stroke can be a manifestation of NBD. It is also important to remember that patients with BD are at higher risk of cardiovascular events including stroke, independent of whether they have NBD.33 Arterial dissections and bleeds, albeit relatively rare in NBD, should trigger suspicion of it in the appropriate clinical setting.
Psychiatric NBD is a rare manifestation, usually with a subacute, progressive presentation, and has highly diverse manifestations, mimicking primary degenerative dementia, depression or frank psychosis. It is very important to consider NBD in such patients.34
An important aspect of the differential diagnosis is the development of a neurological problem in a patient with established BD. The clinicians need to establish whether or not the problem is related to NBD. Besides stroke, headache is a very common complaint in people with BD and it does not generally represent a manifestation of NBD. Vigilance is needed, however, as headache often heralds other manifestations of NBD.
Peripheral neuropathy occurs rarely as a clinical manifestation of NBD and when diagnosed in a person with BD and no other neurological manifestations, a search for alternative aetiologies is warranted.35
Finally, an emerging differential diagnosis aspect concerns neurological complications of BD treatment. It is critical not to mistake such complications for the development of NBD. The role of cyclosporine in NBD is important as it has been linked consistently to a potential acceleration and worsening on NBD. Other treatments also may have complications. Immunosuppressive agents may occasionally facilitate meningitis, which can be confused for NBD. The use of anti-TNF agents such as infliximab, which has been shown to be successful in NBD,36 should require vigilance, as demyelination and other neurological complications have been reported with these agents, although none yet has been reported with use in BD.
Thalidomide, which is occasionally used for BD, predictably causes a neuropathy which is not related to NBD. Posterior reversible encephalopathy syndrome has been reported as a complication of several immune therapies including anti-TNF agents, and at the 2017 CONy symposium, an interesting case in BD was reported by Dr George Vavougios from Greece (Oral communication, CONy Congress, Athens 2017).
In conclusion, NBD is a serious neuroinflammatory condition which poses major diagnostic, differential diagnostic, and therapeutic challenges. Awareness of its clinical features and therapeutic possibilities together with early diagnosis are essential in the management of NBD.







