Introduction
Of the estimated 10 million people worldwide who live with Parkinson’s disease (PD),1 over half will be expected to develop psychosis (hallucinations, illusions, delusions, or a false sense of presence).2,3 Pimavanserin (NUPLAZID®; ACADIA Pharmaceuticals Inc., San Diego, CA, USA) is an atypical antipsychotic developed for the treatment of hallucinations and delusions associated with PD psychosis (PDP).4 Pimavanserin acts as an inverse agonist/antagonist of the serotonin 5-HT2A receptors, and to a lesser extent serotonin 5-HT2C receptors.4 Unlike other atypical antipsychotics, it has no appreciable effect on dopaminergic receptors,4 which are central to the hallmark motor function symptoms of PD, or on muscarinic, histaminergic, or adrenergic receptors.4
The efficacy and safety of pimavanserin was demonstrated in a pivotal, phase III, randomized, placebo-controlled clinical trial (n=199) published in 2014.5 Patients with PDP who received pimavanserin 34 mg/d (equivalent to 40 mg pimavanserin tartrate) for 6 weeks, experienced a significant improvement in psychotic symptoms compared with placebo (3.06-point improvement in the PD-adapted Scale for the Assessment of Positive Symptoms [SAPS-PD] score;6 p=0.001), with no significant safety concerns or worsening of motor function reported relative to placebo.5 Although the incidences were low, an increase in serious adverse events (SAEs) was reported, with 11% (n=11) of patients in the pimavanserin group and 4% (n=4) of patients in the placebo group reporting a SAE, and three deaths occurring during the study: two in the pimavanserin group (sepsis and septic shock) and one in the placebo group (sudden cardiac death).5 Following this, in 2016 the US Food and Drug Administration (FDA) approved pimavanserin as the first antipsychotic indicated for the treatment of PDP with a Breakthrough Therapy Designation, considering the risks to be in line with those of other antipsychotics currently being used off-label in this patient population.4,7,8
However, in November 2017 the Institute for Safe Medical Practices reviewed pimavanserin based on the FDA Adverse Event Reporting System (FAERS). They reported that, since its approval in 2016, a total of 2,236 adverse event (AE) reports had been filed relating to pimavanserin, and of these reports, 244 (10.9%) were for deaths.9 However, it is important to realize that the FDA acknowledges on the FAERS website that there are limitations to the data and interpretation of the data. Since FAERS only reports the total number of events, there is an unclear incidence/prevalence since exposure is not reported. There is also the possibility of duplicate reports, no established causation, and the information has not been verified. Following this, CNN published an article presenting some of these data and highlighting that, since the Institute for Safe Medical Practices report, the number of deaths had now risen to over 700.10 This led to a medical editorial published in The Lancet Neurology in May 2018, highlighting the reasons behind the FDA’s decision to approve pimavanserin for the treatment of PDP and the fact that safety concerns are to be expected in a frail elderly population with psychosis as well as advanced PD.7 Overall, the authors recommended further randomized trials to examine the relative risk of pimavanserin compared with other (off-label) antipsychotic treatments.7
Here we present the highlights of a Spotlight Debate session held at the 23rd World Congress on Parkinson’s Disease and Related Disorders, discussing whether or not the potential increased mortality risk in patients with PDP receiving pimavanserin should be a cause for concern.
Yes, we should worry that pimavanserin might increase mortality amongst patients with Parkinson’s disease and psychosis
Daniel Weintraub
University of Pennsylvania School of Medicine, Philadelphia, PA, USA
|
“The risk–benefit ratio needs to be assessed at an individual patient level when initiating any antipsychotic therapy in patients with PDP or dementia. You have to weigh the benefit of reducing psychotic symptoms against any potential morbidity and mortality associated with treatment… one also needs to consider that PDP has an increased risk of mortality itself, as well as increased institutionalization risk, caregiver burden, and impaired quality of life.” “Outside of the FDA black box warning, there is no clinical trial evidence that would lead one to have any specific concerns at this time about prescribing pimavanserin in patients with PDP.” Daniel Weintraub |
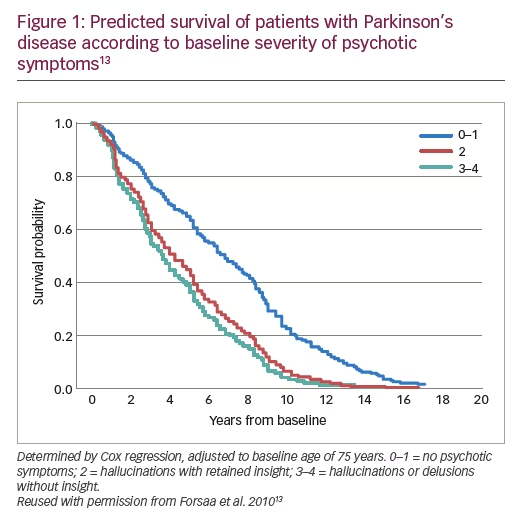
There are several key points that should be considered when assessing the mortality risk of any antipsychotic treatment for PDP. Firstly, patients with PDP already have an inherently higher mortality and long-term morbidity risk compared with PD without psychosis. Studies have shown that hallucinations confer a 2.5-fold increase in the relative risk of nursing home admission,11 that psychosis is one of the most significant causes of repeated and prolonged hospital admissions (accounting for 24% of all admissions in patients with PD),12 and that the presence of psychosis is associated with a significant increase in mortality risk (hazard ratio [HR]: 1.45, 95% confidence interval [CI] 1.02–2.07; p=0.039).13 Indeed, even in patients experiencing less severe psychosis (e.g. two hallucinations with retained insight, or 3–4 hallucinations or delusions without insight), the mortality rate can still be as high as 40% at 3 years and 80% at 7 years (Figure 1).13
Secondly, antipsychotic treatments in general are associated with an increased risk of morbidity and mortality in patients with dementia, e.g. those with Alzheimer’s disease. Following evidence that antipsychotic use in patients with dementia increased the risk of cerebrovascular AEs, and caused a 1.7-fold increase in mortality risk secondary to cardiovascular events and infections, the FDA issued a black-box warning for all atypical antipsychotics in 2005.14 This was then extended to cover typical antipsychotics in 2008.15 This is a particularly important consideration, as PDP is highly associated with cognitive impairment and dementia.16 A study by Aarsland et al. showed that one or more psychiatric symptoms were present in 83% of patients with PD and dementia, with both hallucinations and delusions occurring in a larger percentage of patients with dementia versus those without (54% versus 14% and 29% versus 7%, respectively).16
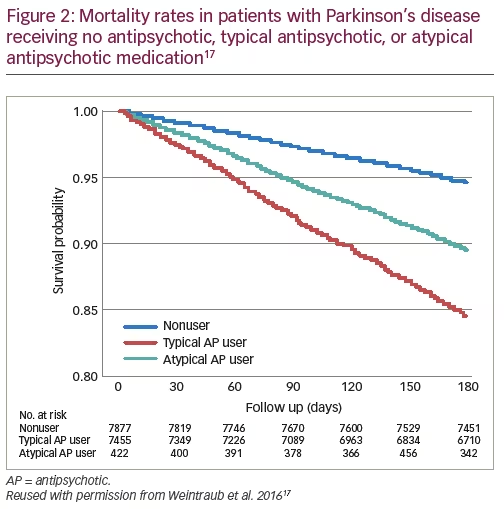
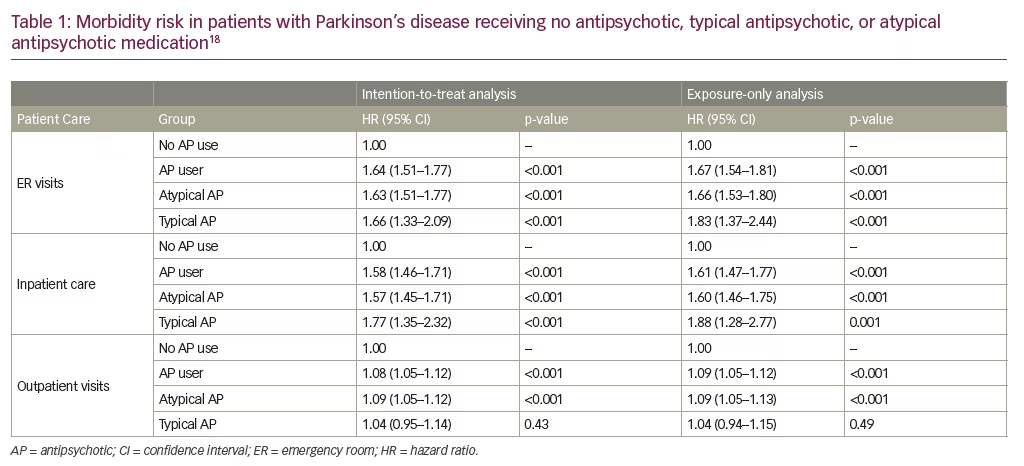
Lastly, recent publications have reported an increased risk of mortality in all patients with PD, not just those with PDP.17,18 In a retrospective, 6-month, matched-cohort study of 15,754 patients with PD from the US Veterans Health Administration database, any antipsychotic use was found to significantly increase the risk of mortality compared with no use (HR: 2.35, 95% CI 2.08–2.66; p<0.001) after adjusting for measurable confounders.17 This trend was true for both typical and atypical antipsychotic use (HR: 3.65 and 2.26, respectively; both p<0.001).17 Typical antipsychotic use was also found to significantly increase the mortality risk compared with atypical antipsychotic use (HR: 1.54, 95% CI 1.24–1.91; p<0.001).17 Overall, the 6-month mortality rates in PD were approximately 5% for patients receiving no antipsychotic therapy, 10% for those receiving atypical antipsychotics, and 15% for those receiving typical antipsychotics (Figure 2).17 Fewer than 10% of the patients in the study were diagnosed with dementia, demonstrating that the increased mortality risk was applicable to patients with PD in general.17 With regard to morbidity, any antipsychotic use was also found to significantly increase the risk of emergency room visits (HR: 1.64, 95% CI 1.51–1.77; p<0.001), inpatient care (HR: 1.58, 95% CI 1.46–1.71; p<0.001), and outpatient visits (HR: 1.08, 95% CI 1.05–1.12; p<0.001) (Table 1).18 Overall, considering these and the previous key points, it is reasonable to be concerned about the use of any antipsychotic in patients with PDP.
In conclusion, there is evidence that pimavanserin might indeed increase mortality in patients with PDP. However, these patients already have an increased morbidity and mortality risk, and all atypical antipsychotics are known to increase the mortality risk in general dementia (and PDP is associated with dementia) as well as in typical PD without dementia.14 In addition, there is a lack of evidence from randomized controlled trials to suggest that pimavanserin is associated with any greater risk than other antipsychotics. A recent study in patients with dementia (Alzheimer’s disease) and psychosis showed pimavanserin to have an acceptable tolerability profile with no detrimental effect on cognition or motor function.19
Nevertheless, the recent articles in the popular press and scientific journals do raise important questions that need to be addressed.7,10 Further research is therefore warranted to characterize the risk–benefit profile of pimavanserin in PDP, in the form of either (i) a large, prospective randomized controlled trial; or (ii) a large-scale, well-designed, case-control study using healthcare claims databases such as Medicare, the US Veterans Health Administration, and national European databases once pimavanserin is available in Europe. <span class="End-box—under-letter"
No, we should not worry that pimavanserin might increase mortality amongst patients with Parkinson’s disease and psychosis
Zoltan Mari
Cleveland Clinic Lou Ruvo Center for Brain Health, Las Vegas, NV, USA
|
“From a scientific perspective, the quality of data from public reporting [such as the FAERS] cannot match the quality and reliability of data from carefully-designed, randomized clinical trials. Also, causality is not possible to evaluate in public reporting… As such, I don’t believe a clear cause–effect relationship has been established between pimavanserin and increased mortality in patients with PDP.” “The distribution mechanism of pimavanserin, with a very direct connection between pharmacies and patients/caregivers, makes it much easier to report AEs and almost certainly has impacted the frequency of adverse events reported.” Zoltan Mari |
While risk of adversity exists with any medication, and such risk must always be carefully considered, it is critical to consider the possible adverse reactions and side effects of treatments relative to the benefits and possible alternatives.
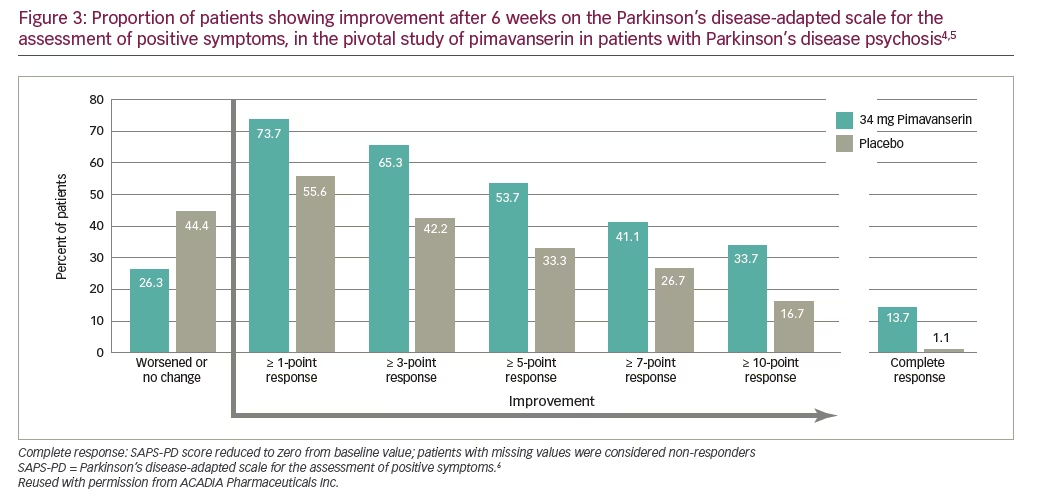
Currently there is neither an approved alternative therapy to treat PDP nor compelling evidence that any other antipsychotic is superior to pimavanserin in terms of efficacy or mortality risk. As mentioned previously, there is a general concern over the increased mortality risk associated with any antipsychotic use in a frail elderly population such as those with PD or dementia,14,15,17,18 and pimavanserin is no exception. However, pimavanserin is the only antipsychotic currently available that has no potential for dopaminergic receptor blocking,4 which could worsen the motor symptoms of PD. This has been demonstrated in preclinical studies as well as both phase II and phase III clinical studies of pimavanserin in PDP, where no treatment-related impairment of motor function has been observed.5,20 It has also been noted that in the pivotal clinical trial, pimavanserin showed only a 3-point improvement over placebo on the SAPS-PD scale in patients with PDP.5 Importantly, a 2.33-point change in the SAPS-PD has been correlated with a clinically meaningful 1-point change in the clinical global impression – improvement scale.6 However, it should be remembered that this represents a mean population value and was statistically significant (p=0.001; Cohen’s d=0.50),5 with 73.7% of patients experiencing an improvement of ≥1 point on SAPS-PD (compared with 55.6% in the placebo group) and 33.7% reporting improvements in excess of 10 points in the pimavanserin group (compared with 16.7% in the placebo group; Figure 3).4,5 To place such improvements in context, patients who received pimavanserin had a mean SAPS-PD change after 6 weeks that equated to a 37% improvement from baseline in SAPS-PD, compared with 14% for placebo.5 Overall, the benefits of pimavanserin in patients with PDP are both statistically and clinically significant, and pimavanserin is the only antipsychotic that demonstrates these benefits with no associated clinical activity on dopamine receptors.
With regard to the post-marketing safety reports detailed in the popular press and scientific journals,7,10 there are two important points that should be considered. Firstly, without professional data forms or controls there is no reliable way of determining causality with FDA public reporting via FAERS, particularly in a PDP population that is typically elderly and frail, with multiple cognitive and medical comorbidities and various causes of death unrelated to pimavanserin. In addition, no consistent pathology or pattern of treatment-related AEs was observed in the pivotal clinical trial of pimavanserin in PDP,5 and currently there is no known pharmacological mechanism related to pimavanserin that might explain the majority of SAEs or deaths reported in FAERS.
To complement safety monitoring during the preclinical and clinical development of pimavanserin, ACADIA initiated all required post-marketing surveillance of product safety. In addition, pimavanserin was distributed via specialty pharmacies and specialty distributors that enabled frequent contacts with patients and caregivers, during which they were able to report AEs far more readily and easily than is standard. This, combined with the naturally heightened interest associated around a new drug with a novel mechanism of action, clearly enhanced the scrutiny towards AEs. It was expected that more frequent patient/caregiver contacts would generate a larger number of AE reports, and it is estimated that since the beginning of 2017, approximately 85% of all AE reports have been received via these contacts.21
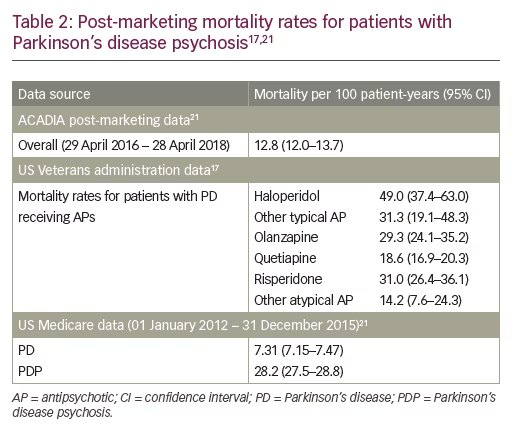
Because of the unknown reliability of uncontrolled data, it seems pertinent to focus on safety data from clinical trials when assessing the benefit-risk profile of pimavanserin. At approval (April 2016) the crude mortality rates from placebo-controlled studies of pimavanserin in PD/PDP were 0.7% (3/420; 7.0 per 100 patient-years [PY]) and 0.4% (1/266; 3.6 per 100 PY) for pimavanserin and placebo, respectively.5,20–22 This does indeed show an almost 2-fold increase in mortality with pimavanserin. However, the overall numbers of deaths were very low and this can be attributed to chance. As of April 2018, when more data became available from placebo-controlled clinical studies (including one study in patients with Alzheimer’s disease psychosis),19 the crude mortality rates were similar for both pimavanserin and placebo (1.2% [6/510; 10.0 per 100 PY] and 1.4% [5/357; 10.9 per 100 PY], respectively).21 These compare favorably with the crude mortality rates previously reported for antipsychotic treatments from 15 placebo-controlled studies in patients with dementia (antipsychotics: 3.5% [118/3,353; 20.7 per 100 PY]; placebo: 2.3% [40/1,757; 13.2 per 100 PY]).23 Similarly, post-marketing mortality rates in patients with PD receiving other typical and atypical antipsychotics range from 14.2–49.0 per 100 PY,17 whereas pimavanserin post-marketing data show an overall mortality rate of 12.8 per 100 PY (Table 2).21 In addition, the age-standardized mortality rate for patients with PDP based on US Medicare data (January 2012 to December 2015) is also substantially greater (28.18 per 100 PY) than that reported for patients receiving pimavanserin (Table 2).21
In conclusion, while we should always be concerned about the risks associated with any treatment, available evidence from controlled studies indicates that the risks associated with pimavanserin are no worse than those associated with other antipsychotics in patients with PDP, with the added benefit that pimavanserin has no dopamine receptor blocking activity that could potentially worsen the motor function symptoms of PD.
Summary
Overall, while the FDA FAERS data might indicate an increase in mortality, the causality of this increase is not clearly established. Reflecting this, the FDA recently released a statement based on the results of a review of all post-marketing reports of deaths and SAEs in patients receiving pimavanserin, which concluded that the post-marketing safety data were consistent with the pre-marketing clinical trial data, and that the benefits of pimavanserin outweigh the risks for patients suffering hallucinations and delusions associated with PDP.24 Further research in the form of randomized, controlled trials and large-scale pharmaco-epidemiological studies, in contrast to the post-marketing data to date, is required to fully characterize the risk–benefit profile of pimavanserin. Nevertheless, as the only currently-approved treatment, pimavanserin addresses an important unmet clinical need in patients with PDP, a condition with psychotic symptoms that, if left untreated, can have a substantial impact on patient quality of life and caregiver burden.







