Management of neuropathic pain is a real clinical challenge. Current treatments focus on blocking neurotransmission and do not differentiate between different phases of neuropathic pain pathophysiology. The authors have recently shown that nerve-injury-induced neuropathic pain development requires matrix metalloprotease-9 and -2 (MMP-9 and MMP- 2) in the early and late phase, respectively. Inhibition of MMP-9 or MMP-2 may provide a novel therapeutic approach for the treatment of neuropathic pain at different phases.
Neuropathic Pain Symptoms and Mechanisms
Management of neuropathic pain is a real clinical challenge. Current treatments focus on blocking neurotransmission and do not differentiate between different phases of neuropathic pain pathophysiology. The authors have recently shown that nerve-injury-induced neuropathic pain development requires matrix metalloprotease-9 and -2 (MMP-9 and MMP- 2) in the early and late phase, respectively. Inhibition of MMP-9 or MMP-2 may provide a novel therapeutic approach for the treatment of neuropathic pain at different phases.
Neuropathic Pain Symptoms and Mechanisms
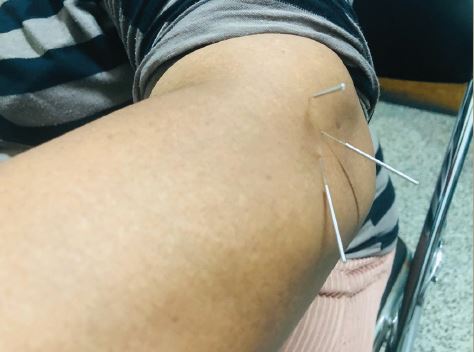
Many patients in the pain clinic suffer from neuropathic pain due to injury to the peripheral nervous system (PNS) (e.g. peripheral nerves) or the central nervous system (CNS) (e.g. spinal cord and thalamus). These injuries may result from major surgeries (e.g. amputation and thoracotomy), diabetic neuropathy, viral infection, chemotherapy, spinal cord injury, stroke, and so forth. Although neuropathic pain in animal models after specific nerve injury is highly reproducible, only a portion of patients after nerve injuries will develop neuropathic pain, depending on genetic background and medical history.1 Neuropathic pain is often characterized by spontaneous pain, described as shooting, lancinating, or burning pain, and also by evoked pain, such as hyperalgesia (increased responsiveness to noxious stimuli) to mechanical and thermal stimuli. Probably the most distinct symptom of neuropathic pain is mechanical allodynia (painful responses to normally innocuous tactile stimuli). For example, patients feel enormous pain during movement. Currently available drugs such as tricyclic antidepressants, anticonvulsants, sodium channel blockers, N-methyl-D-aspartate (NMDA) receptor antagonists, and opioids provide relief from neuropathic pain in only a fraction of such patients, with severe side effects.2,3 This failure results in part from the strategy of these drugs to block neurotransmission, ignoring the underlying pathology of neuropathic pain. Therefore, pain relief after many treatments often lasts no longer than the drug’s presence at the site.
Neuropathic pain research has been accelerated with different animal models in which the sciatic nerve and its branches, or the spinal nerves, or the spinal cord are intentionally damaged.1,4 How well these different injury models include the clinically presenting pain syndromes remains an important concern for validating common mechanisms and establishing animal models for human drug testing. However, clinical cases are often difficult to study because there are multiple contributing factors and the time from the initial insult, when it is recognized, can vary from several days, to weeks, to years. Thus, most mechanistic studies are based on animal models.
Mechanisms of neuropathic pain are incompletely known. Neural mechanisms of neuropathic pain have been extensively investigated over several decades. It is generally believed that neuropathic pain manifests as an expression of neural plasticity both in the PNS (peripheral sensitization) and CNS (central sensitization). Central sensitization in spinal cord dorsal horn neurons is particularly important for the persistence of neuropathic pain and spread of pain beyond the initial injury site. Central sensitization in dorsal horn neurons can be induced both by an increase in excitatory synaptic transmission mediated via the glutamate NMDA and alpha-amino-3-hydroxy-5-methyl-4- isoxazolepropionic acid (AMPA) receptors and a decrease or loss of inhibitory synaptic transmission (disinhibition) mediated via gamma-aminobutyric acid (GABA) and glycine receptors.2
Increasing evidence has also suggested glial mechanisms of neuropathic pain. Nerve injury induces a profound activation of glial cells such as microglia and astrocytes in the spinal cord, and the activated glia can release multiple pain mediators to enhance neuropathic pain via glial–neural interaction.1,5,6 For example, peripheral nerve injury induces very dramatic changes in spinal cord microglia and astrocytes, including morphological changes, proliferation, and upregulation of the glial markers (e.g. CD11b/OX-42, Iba1, and glial fibrillary acidic protein [GFAP]). Several glial inhibitors, such as flurocitrate, alpha-aminoadipate, minocycline, and propentofylline, have been shown to attenuate neuropathic pain.5,7 In particular, mitogen-activated protein kinases (MAPKs) are activated in glial cells after nerve injury and serve as critical signaling molecules in glia for neuropathic pain sensitization. MAPK activation in glial cells may lead to the production of inflammatory mediators such as prostaglandins, cytokines, and chemokines, as well as growth factors, to enhance and maintain neuropathic pain.1,8–10
Pro-inflammatory cytokines such as interleukin (IL)-1β, IL-6, and tumor necrosis factor (TNF)-α are produced after nerve injury and play an essential role in neuropathic pain sensitization.1,5,11,12 First, they are produced in the damaged nerve tissue by Schwann cells or infiltrating immune cells and have been shown to increase the sensitivity and excitability of sensory neurons by activating the TTX-resistant sodium channels Nav1.8 or capsaicin receptor TRPV1. Second, they are produced by glial cells in the spinal cord and directly enhance synaptic transmission in nociceptive neurons in the spinal cord. For example, TNF-α and IL-6 can enhance excitatory synaptic transmission and suppress inhibitory synaptic transmission, respectively, in dorsal horn neurons. In contrast, IL-1β is more dynamic: it not only increases excitation but also decreases inhibition.12 These cytokines can also produce long-term effects on synaptic plasticity by inducing gene transcription.12 However, how these cytokines are activated after nerve injury is unclear. IL-1β is synthesized as a precursor (31kDa) and subsequently cleaved into a partially processed form (28kDa) and a completely processed or mature form (17kDa). The precursor form of IL-1β shows little or no biological activity. Intracellular IL-1β consists exclusively of the precursor form. Although caspase-1, also known as IL-1β-converting enzyme, is a well-documented protease for IL-1β activation, other enzymes such as trypsin, elastase, collagenase, and metalloprotease are also implicated in IL-1β cleavage.13 It is worthwhile to mention that under several inflammatory conditions, caspase-1-deficient mice can still mediate IL-1β-dependent reactions and produce the same level of bioactive IL-1β.14
Neuropathic Pain Phases
Different phases of neuropathic pain have not been clearly defined so far, and these phases may vary under different injury conditions. However, there are at least two phases in animal models: an early phase (first several days) when neuropathic pain is developed, and a late phase (from a week to months and even years) when neuropathic pain is maintained. It appears that, after nerve injury, microglia activation (e.g. upregulation of the microglial markers CD11b and Iba1) in the spinal cord peaks in the early phase but declines in the late phase, as does the activation of p38 MAPK in spinal microglia.9 Therefore, the analgesic efficacy of spinal injection of p38 inhibitor reduces in the late phase.8 Furthermore, minocycline, a microglial inhibitor, attenuates neuropathic pain in the early phase but not in the late phase.7 In contrast, astrocyte activation (e.g. upregulation of the astrocyte markers GFAP and S-100) remains at the peak level even in the late phase. Several signaling molecules such as phophorylated c-Jun N-terminal kinase (pJNK) and basic fibroblast growth factor (bFGF) are persistently upregulated in spinal cord astrocytes. Consistently inhibiting astrocytes with several inhibitors such as alpha aminoadipate and JNK inhibitor can very effectively attenuate neuropathic pain in the late phase.9 In particular, the phosphorylated extracellular regulated kinase (pERK) shows dynamic changes in different spinal cell types at different times after nerve injury. First, pERK is induced in dorsal horn neurons in the first several hours of nerve injury, representing an immediate injury-induced neuronal excitation. Second, pERK is switched to microglia after two days (early phase). Finally, pERK is switched to astrocytes in the late phase (one to three weeks). Inhibition of the ERK pathway in the spinal cord in either the early phase or the late phases can very effectively reduce neuropathic pain.10 These sequential changes of pERK expression in different cell types over time strongly indicate that there exist different phases of neuropathic pain. Thus, rapid microglia activation plays an important role in the induction or early-phase development of neuropathic pain, whereas delayed and persistent astrocyte activation contributes to the maintenance or late-phase development of neuropathic pain. However, some very late microglial responses were also obverted after peripheral nerve injury despite peak microglial responses in the early phase. Notably, heat hyperalgesia after nerve injury tends to resolve in several weeks, whereas mechanical allodynia remains for a much longer period. While thermal pain is often restricted to the injury site, mechanical allodynia can spread beyond the initial injury site, even to the contralateral side of the body part (mirror pain), which is controlled by a spinal cord mechanism. A network of astrocytes in the spinal cord may be involved in the spread and persistence of mechanical pain.
Matrix Metalloproteases and Neurological Diseases
MMPs belong to a large family of endopeptidases that require Zn2+ for their enzyme activity. MMPs play a critical role in neuroinflammation through the cleavage of the extracellular matrix (ECM) proteins, cytokines, and chemokines.15–17 There are more than 20 members in the MMP family, consisting of several major classes such as gelatinases, collagenases, stromelysins, and membrane-type MMPs. MMP-2 (gelatinase A) and MMP-9 (gelatinase B) are two of the best-studied MMPs. These are secreted proteins and present in the ECM, cerebrospinal fluid, and serum. The activity of MMP-2 and MMP-9 can be easily detected by gelatinsubstrate zymography. When gelatin is embedded in the eletrophoretic gel, it is digested by the gelatinase MMP-2 and MMP-9. MMP-2 is constitutively expressed and normally present in brain and spinal cord tissues. In contrast, MMP-9 is normally expressed at low levels but upregulated in many injury and disease states such as spinal cord injury and brain trauma.16 MMP-9 is also induced in the crushed sciatic nerve and causes demyelination, a condition associated with neuropathic pain, by the cleavage of myelin basic protein.18 MMP activity is regulated by endogenous inhibitors, called tissue inhibitors of metalloproteases (TIMPs). The activity of MMP-9 and MMP-2 can be inhibited by the formation of tight 1:1 non-covalent complexes with TIMPs, such as the MMP-9/TIMP-1 and MMP-2/TIMP-2 complex.19
In recent years, MMPs have been implicated in a wide range of CNS diseases, including Alzheimer’s, amyotrophic lateral sclerosis, multiple sclerosis, brain and spinal cord trauma, and stroke. By degrading the extracellular matrix in the CNS, MMPs damage the blood–brain barrier, resulting in edema and vascular leakage. By interrupting cell–cell and cell–matrix homeostasis, MMPs can also trigger anoikis-like pathways of brain cell death.15,16,20 Besides targeting matrix, MMPs can process a variety of growth factors and other extracellular cytokines and signals. In this regard, MMPs may contribute to the neurovascular remodeling that accompanies chronic CNS injury.21 Depending on whether functional or dysfunctional remodeling occurs, the result might be recovery or the induction of aberrant neuronal circuits, some of which may be involved in the generation of pain.
Matrix Metalloprotease-9 and Early-phase Neuropathic Pain
Spinal nerve ligation (SNL) at the L5 level is known to produce rapid (less than one day) and persistent (>21 days) neuropathic pain symptoms (e.g. mechanical allodynia) in rats and mice.4,22 The authors used gelatin zymography to check MMP-9 activity and expression in the L5 dorsal root ganglia (DRG) collected from naive animals and injured animals (six hours to 21 days after SNL). SNL induces a rapid (less than one day) but transient (more than three days) upregulation of MMP-9 in the DRG. Furthermore, MMP-9 expression increases in DRG neurons on day one.22 To define the specific role of MMP-9 in neuropathic pain development, the authors employed five different approaches:
• small synthetic inhibitor of MMP-9;
• endogenous peptide inhibitor of MMP-9 (TIMP-1);
• small interfering RNA against MMP-9;
• exogenous MMP-9 injection; and
• MMP-9 knockout mice.
To avoid systemic effects of drugs, the authors delivered these drugs into spinal fluid via intrathecal administration to target MMP-9 in the DRG and spinal cord. Results from these five different approaches are very consistent, showing that MMP-9 inhibition or deletion can attenuate neuropathic pain in the early phase. Conversely, intrathecal injection of exogenous MMP-9 is sufficient to induce mechanical allodynia. In particular, the endogenous inhibitor TIMP-1 is 1,000 times more potent than morphine, a commonly used analgesic to treat neuropathic pain, and the duration of pain suppression by TIMP-1 is also 10 times longer than that of morphine. However, this powerful inhibitor only works in the early phase (e.g. day one), not in the late phase (e.g. day 10).22
The authors have further explored the mechanisms by which MMP-9 induces neuropathic pain. SNL induces a marked IL-1β activation (cleavage) in the DRG in the early phase (day one), which is lost in mice lacking Mmp9, suggesting that MMP-9 is needed for IL-1β activation after nerve injury. Injection of MMP-9 is also sufficient to induce IL-1β activation in the DRG. Furthermore, MMP-9 and IL-1β are co-expressed in the same neurons in the DRG.22 The authors hypothesize that nerve-injury-induced spontaneous discharge in sensory neurons can release MMP-9 and pro-IL- 1β into the ECM, where MMP-9 cleaves pro-IL-1β to produce active IL-1β. The active IL-1β then acts on adjacent nociceptive neurons to produce hyperexcitability. The authors’ behavioral studies show that blocking IL-1β with a neutralizing antibody can suppress neuropathic pain symptoms induced either by MMP-9 or by nerve injury, supporting an important role of the MMP-9/IL-1β cascade in neuropathic pain development. Finally, MMP-9 in DRG soma is transported to central terminals in the dorsal horn to activate microglia. At the spinal level, MMP-9 is sufficient to activate microglia even in a low dose that does not produce demyelination and apoptosis.22 Collectively, MMP-9 induces early-phase neuropathic pain by activating IL-1β and microglia in the early phase.
Matrix Metalloprotease-2 and Late-phase Neuropathic Pain
Nerve injury also induces an upregulation of MMP-2, but the induction pattern of MMP-2 is quite different from that of MMP-9:
• in contrast to a rapid and transient upregulation of MMP-9, SNL produces a delayed (more than seven-day) and persistent (>21-day) upregulation of MMP-2 in the DRG;
• while MMP-9 is induced in DRG neurons, MMP-2 is induced in small satellite cells surrounding DRG neurons; and
• although MMP-9 activity in the spinal cord is low even after nerve injury, in part due to rapid release from central terminals, MMP-2 upregulation is persistently induced in spinal cord astrocytes.22
Satellite cells in the DRG and astrocytes in the spinal cord share some similar features: they both show persistent upregulation of GFAP and pERK after nerve injury and contribute to the maintenance of neuropathic pain. Of interest, MMP-9 is not necessary for MMP-2 upregulation, since SNL still upregulates MMP-2 even in Mmp9 knockout mice.
To determine the role of MMP-2 in late-phase neuropathic pain, three different pharmacological approaches were used:
• small synthetic inhibitor of MMP-2;
• endogenous peptide inhibitor of MMP-2 (TIMP-2); and
• small interfering RNA against MMP-2 to block MMP-2 in the late phase.
The data consistently show that MMP-2 inhibition can very effectively attenuate neuropathic pain in the late phase. In contrast, injection of exogenous MMP-2 is able to induce neuropathic pain symptoms.22 While MMP-9 induces IL-1β cleavage and activation in the early phase, MMP-2 appears to do this in the late phase. MMP-2 is also important for the activation of spinal cord astrocytes, since MMP-2 inhibition can suppress pERK induction in spinal cord astrocytes in the late phase.22 Taken together, MMP-2 contributes to late-phase neuropathic pain development by activating IL-1β and astrocytes in the late phase.
Clinical Significance and Future Directions
Chronic pain affects more than 50 million Americans per year and is widely believed to represent a disease itself. In particular, neuropathic pain is very destructive and current treatments for this pain have only resulted in limited success. This failure results, in part, from the following reasons. First, our knowledge of neuropathic pain development and maintenance is incomplete and current treatments do not differentiate between different phases of neuropathic pain. Second, current treatments often ignore the pathology of neuropathic pain and simply focus on blocking neurotransmission, producing only transient pain relief. The authors’ studies suggest that MMP-9 inhibition may be used to prevent neuropathic pain induced after major surgeries (e.g. amputation, thoracotomy) and trauma (e.g. spinal cord injury), whereas MMP-2 inhibition may be used to treat established neuropathic pain such as diabetic neuropathy.
MMPs belong to a very large family and they can activate each other. It is important to understand a network activation of different MMPs in neuropathic pain conditions. Different MMPs may play different roles in neuropathic pain. Thus, a broad inhibitor of MMPs may not be very effective and will produce severe side effects, since MMPs are involved in tissue remodeling and wound healing.21 However, it is a real challenge to develop highly specific small synthetic inhibitors that only inhibit MMP-9 or MMP-2. More specific targeting of MMP-9 or MMP-2 with monoclonal antibodies, siRNAs, and peptide inhibitors may reduce the side effects of broad MMP inhibitors. Apart from IL-1β, MMP-9 and MMP-2 are likely to cleave multiple substrates to promote neuropathic pain. It is important to investigate the potential substrates in the DRG and spinal cord tissues, which may also lead to novel therapeutics by targeting the interaction between MMP-2/-9 and their substrates. Finally, the tetracycline minocycline is a relatively safe drug and has been proposed to treat different types of neurological diseases. Of interest, minocycline is also an inhibitor of MMP-9.23,24 However, a recent clinical trial testing minocycline in ALS failed.25 This failure may result in part from treating patients in the late phase of disease development. Currently, there is also an ongoing National Institutes of Health (NIH) trial testing minocycline in stroke (David Hess, MCG, Augusta, Georgia, personal communication). Minocycline may also be used to prevent neuropathic pain after trauma and major surgeries. ■