Risk Factors for Psychosis in Parkinson’s Disease
Abstract
Overview
Psychosis is a characteristic neuropsychiatric symptom of Parkinson’s disease (PD) that is common and associated with worse outcomes. The purpose of this article is to review identified risk factors for visual hallucinations in PD, the most common manifestation of psychosis. With the possible exception of dopamine agonists, antiparkinsonian medications are only considered modifiers of psychosis in PD. Dementia in PD has consistently been shown to be associated with psychosis, and executive dysfunction and impairment in visual processing appear to play a role in its pathogenesis. The association of psychosis with disorders of sleep–wake dysregulation and autonomic dysfunction
supports the involvement of brainstem dysfunction in PD psychosis. Despite many studies evaluating genetic risk factors for hallucinations, GBA mutations are the only variants consistently reported to be associated with an increased risk of hallucinations in PD. Lastly, psychosis in PD is
associated with a more severe disease burden, both related and unrelated to PD pathology. Any explanatory model of psychosis in PD must incorporate pharmacological, neuroanatomic, pathological, and genetic factors before there can be a complete understanding of this common
and disabling neuropsychiatric symptom.
Keywords
Parkinson’s disease, psychosis, hallucinations, risk factor, dementia, rapid eye movement (REM) sleep behavior disorder
Article Information
Disclosure
Matthew J Barrett has received grant support from the Department of Defense and the Commonwealth of Virginia’s Alzheimer’s and Related Diseases Research Award Fund and has served as site primary investigator for clinical trials funded by the National Institutes of Health, Azevan, Axovant, and Merck. No funding was received in the publication of this article.
Authorship: All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship of this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval to the version to be published.
Correspondence
Matthew J Barrett, University of Virginia, Department of Neurology, PO Box 800394, Charlottesville, VA 22908, US. E: mjbarrett@virginia.edu
Access
This article is published under the Creative Commons Attribution Noncommercial License, which permits any non-commercial use, distribution, adaptation and reproduction provided the original author(s) and source are given appropriate credit.
Received
2017-05-22T00:00:00

Trending Topic
Article highlights Multiple screening tests are available to screen patients for cognitive impairment, and the Confusion Assessment Method is a helpful test to screen for delirium in the immediate postoperative period. Medicine reconciliation and identification and removal of potentially inappropriate medications per Beer’s list are important tasks that should not be overlooked, especially during a preoperative appointment. […]
Related Content in Psychiatric Disorders

While Alzheimer’s disease (AD), the most common cause of dementia, is perhaps best characterized by cognitive decline, more than 90% of patients with dementia exhibit behavioural and psychological symptoms of dementia.1 The Cache County Study on Memory in Aging describes ...

Postpartum depression (PPD) is an important mental health problem that is associated with maternal distress and poor maternal–fetal bonding. The Diagnostic and Statistical Manual of Mental Disorders (DSM-5) now classifies PPD as major depressive disorder (MDD), with peripartum onset.1 ...

Parkinson’s disease (PD) is a progressive, neurodegenerative movement disorder and the second most common neurodegenerative disorder in the United States.1 In 2020, approximately 930,000 people in the United States aged 45 years and older developed the disease, and this number is expected ...

Multiple sclerosis (MS) is a chronic neurological disease that is associated with high rates of depression and anxiety,1 particularly in the early stages of diagnosis.2,3 A growing body of evidence suggests that cognitive behavioural therapy (CBT) is an effective treatment ...

Altered neurotransmission of γ-aminobutyric acid (GABA) has been implicated in the pathogenesis of depression. In this expert interview, Dr. Handan Gunduz-Bruce discusses the background and rationale for investigating zuranolone, an oral, positive allosteric modulator of GABA type A (GABAA) receptors, ...

Pathologically, Parkinson’s disease (PD) is characterized by the loss of dopaminergic neurons in the substantia nigra and the presence of Lewy bodies.1 In a staging model proposed by Braak in 2003,2 the presence of midbrain lesions are preceded by degeneration ...

Parkinson’s disease (PD) has been traditionally defined by the motor symptoms of bradykinesia, resting tremor, rigidity and postural instability;1 however, more recently, it has been recognized that neuropsychiatric symptoms such as psychosis, anxiety, depression, apathy, impulse control disorders and ...
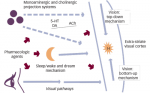
Parkinson’s disease (PD) is a progressive neurodegenerative synucleinopathy. Clinical diagnosis is based on the presence of motor symptoms, including bradykinesia, rigidity, rest tremor, and postural instability.1 Although the cause of PD is still unknown, the severe nigro-striatal dopamine loss ...

In the field of clinical psychopharmacology, substantial progress has been made in the drug treatment of schizophrenia with the advance of novel/atypical antipsychotics. Neuroleptic medication is the most important part of the treatment regimen for schizophrenic patients. The efficacy ...

Niemann-Pick disease type C (NPC) is a rare and fatal neurovisceral lipid storage disorder that affects both children and adults. Whereas the disease in children is characterised by mental retardation, seizures and often rapid neurodegeneration, in adults the disease is ...

Kynurenine is further metabolized along two distinct routes: the kynurenine–kynurenic acid (KYNA) pathway, regulated by kynurenine amino transferase (in both astrocytes and microglia) and resulting in production of KYNA, the only known endogenous N-methyl-D-aspartic acid (NMDA) antagonist; and the ...

Clinical Features of Progressive Supranuclear Palsy Clinical Features of Progressive Supranuclear Palsy Progressive supranuclear palsy (PSP) is a neurodegenerative disorder characterised by parkinsonism, supranuclear ophthalmoplegia, dysphagia and cognitive dysfunction. The National Institute of Neurological Disorders and Stroke (NINDS) PSP criteria ...
Latest articles videos and clinical updates - straight to your inbox
Log into your Touch Account
Earn and track your CME credits on the go, save articles for later, and follow the latest congress coverage.
Register now for FREE Access
Register for free to hear about the latest expert-led education, peer-reviewed articles, conference highlights, and innovative CME activities.
Sign up with an Email
Or use a Social Account.
This Functionality is for
Members Only
Explore the latest in medical education and stay current in your field. Create a free account to track your learning.

