The syndrome has attracted even more interest recently as it has been recognised as an independent cardiovascular risk factor and studies on the treatment of OSAS have postulated a risk reduction of fatal and non-fatal cardiovascular events.5,6 Nonetheless, it is estimated that 90% of people with the condition remain undiagnosed.7 Therefore, the primary objective of clinical pre-test evaluation and overnight testing should focus on a timely, cost-effective and targeted diagnostic approach to identify those who will benefit from treatment. Ideally, diagnosis would lead physicians to identify those patients with potential benefit from treatment and avoid trying it on those who will not.8 Focusing on symptoms rather than respiratory parameters may better address outcome parameters that are relevant for patients, which should be adopted as the gold standard of OSAS diagnosis instead of number counts of respiratory-disturbance parameters, oxygen dip rates or arousals.
Pre-test Evaluation for Suspected OSAS
Patient History
The diagnosis of OSAS is first suspected on clinical grounds based on a typical history. Patients complain of non-restoring sleep, daytime fatigue and sleepiness, and sometimes even sleep attacks. Sleepiness is frequently reported in situations of reduced attention, such as driving on motorways, and at times of rest or inactivity. Some patients also complain of morning symptoms such as headache and fatigue; others suffer from mood disturbance. Loud snoring, apnoeas and gasping or choking are witnessed by bed partners. Notably, partners often ask patients to seek medical help because they better recognise the loss of attention, concentration and interest, as the disease evolves gradually and patients become accustomed to their sleepiness, unaware of their evolving symptoms. Some patients even report previous workplace or driving accidents, or near-misses. Quality of life and social contacts are often seriously impaired. Subjective rating tests of sleepiness include the Epworth Sleepiness Scale, Profile of Mood States and the Stanford Sleepiness Scale.9–11 Of these, the Epworth Sleepiness Scale is most commonly used as, in different studies, a more significant effect on the extent of impairment with OSAS was shown compared with normal subjects.12,13 Impaired-health-related quality of life may be assessed by the SF-36 questionnaire.14 Clinical Findings
Middle age and male gender are strong predictors of OSA.15 Although the male predisposition of airway collapse in sleep has been known for some years, patho-anatomic and pathophysiological reasons for this are not fully elucidated.16–19 Many patients with OSAS have an anatomically small airway due to obesity, enlarged tonsils and adenoids or narrowing by bony structure such as retrognathia.20 A high Mallampati score, which is assessed by simple inspection of the oral cavity, represents an important predisposing factor for OSAS.21 Neck circumference has been shown to correlate even more strongly with oxygen-saturation dip rates than general obesity, which itself is also a significant predictor for OSAS.15,22 A variety of upper-airway imaging modalities have shown potential to gain insight into the pathogenesis of sleep apnoea and prediction of successful treatment outcomes, but are not yet routinely part of the basic diagnostic approach in most sleep laboratories.23 Arterial hypertension is common, the association of OSAS with hypertension having been demonstrated with large, population-based studies.24 As a consequence of nocturnal sympathetic activation, the normal night-time ‘dipping’ of blood pressure is blunted.25 If this is suspected, 24-hour blood-pressure monitoring is recommended.
Tests for Cognitive Performance
Objective assessment of cognitive performance in OSAS can be conducted with a variety of tests that are capable of assessing for attention, memory and learning, as well as planning skills and problem solving. Relevant impairment of all cognitive areas has been documented in population-based studies, including patients with an AHI as high as 30/h.26 However, effects of OSAS on sleepiness seem to be higher than on cognitive dysfunction, which was also supported by experimental evidence.27
Objective Tests for Sleepiness
Sleepiness can be quantified to some extent by polysomnographic tests – the Multiple Sleep Latency Test (MSLT) and the Maintenance of Wakefulness Test (MWT).28 During the MSLT, the subject’s tendency to fall asleep during four daytime nap opportunities is measured, while the MWT tests the subject’s capability to stay awake for as long as possible in repetitive trials in a darkroom. Both the MSLT and MWT do not discriminate well between patients with sleep disorders and the normal population, but both tests show appropriate changes between pre- and post-treatment testing and subsequent testing after manipulations intended to alter sleepiness or alertness. Additionally, the presence of two or more sleep-onset rapid-eye-movement periods in the MSLT is a common finding in narcolepsy patients.28
Daytime vigilance can also be measured by the Oxford Sleep Resistance (OSLER) test.29,30 The OSLER test and environment are comparable to the MWT. The mean time until seven successive responses to a light signal of three seconds are missed and the mean number of missed stimuli per minute are recorded during four test sessions on the same day.31 As a most important advantage, the test can be performed unattended with no electroencephalogram (EEG) electrodes attached, making it a less expensive and less time-consuming option.
Measurement Techniques for Respiratory Disturbance in Sleep
Polysomnography
The confirmation of the OSAS diagnosis requires the documentation of sleep-related breathing disturbances. According to current standards this is performed by polysomnography, an overnight study in a quiet room using techniques to assess sleep and wakefulness – electroencephalography, electro-oculography and electromyography. Simultaneously, cardiorespiratory function (i.e. air flow, chest-wall motion, pulse oximetry, electrocardiogram (ECG)) is monitored. Nasal air flow is best measured with a nasal cannula, and thoraco-abdominal movement with inductive respiratory plethysmography (RP).32 Audiovisual recordings are included in most studies and polysomnography is supervised by a technician.
Analysis requires tedious manual scoring; however, the technique has indisputable merits and advantages compared with limited diagnostic systems. With the inclusion of an EEG, sleep disruption caused by apnoeas and hypopnoeas and even more subtle respiratory effort-related arousals are registered. The average number of apnoeas and hypopnoeas occurring per hour of sleep are commonly referred to as the AHI or RDI. Periodic limb movements are also routinely recorded with EMG electrodes to the fibular muscles. Limb movements may provoke repeated arousals, which are easily recognised on the EEG and may also cause daytime sleepiness. However, in patients evaluated for OSAS periodic leg movements are often incidental findings and are unlikely to contribute to daytime fatigue and sleepiness.33 With the custom addition of video surveillance, even more information is taken from in-laboratory sleep studies, e.g. the occurrence of parasomnias, epilepsy or sleep choking. In ‘split-night’ studies, the night is split in two: the first half is for diagnosis and the second half is used for supervised nasal continuous positive airway pressure (nCPAP) titration. Polysomnography is therefore regarded as the gold standard for the diagnosis of OSAS by many authorities. Several studies have shown that variables derived from polysomnography cannot accurately predict which patients will benefit from CPAP therapy and polysomnography has not been proved to be any more accurate and cost-effective than limited cardiorespiratory monitoring (CRM) in a randomised trial.34,35 Moreover, it remains unclear which level of severity of sleep-disordered breathing recorded during a polysomnography warrants treatment. Thus, symptomatic patients with mild to moderate OSAS (AHI 5/h–30/h) have experienced improvements in sleepiness and other outcomes. Conversely, asymptomatic subjects with high AHIs (>30/h) did not improve their quality of life, symptoms, objective vigilance or blood pressure during CPAP therapy.36 This may be explained in part by a lack of strong relationships between conventional nocturnal measures such as arousals or respiratory events and daytime function in patients with OSAS.37
CRM
Access to polysomnography has been restricted due to its cost and limited availability,38 which has been recognised by US and European experts.39 Bearing in mind the evidence that untreated sleep apnoea is deleterious to patients and expensive to the healthcare budget,40,41 limited in-laboratory and even portable home-based sleep study devices, henceforth CRM, have emerged. Other terms that have been used instead of CRM include portable diagnostic system, portable monitoring device, modified portable sleep apnoea testing or type-3 monitors. CRM incorporates a minimum of four channels, including signals of air flow (at least two channels of respiratory movement or respiratory movement and air flow, measured with thermistors or pressure curves as surrogates of air flow), heart rate or ECG, and oxygen saturation. Some CRM devices also register snoring sounds, body position and leg movements. CRM may be performed attended or unattended in a hospital room or as an outpatient study in the patient’s home, which offers a potential advantage in terms of improved sleep quality in the patient’s habitual environment.42
In 2003, a systematic review identified 12 studies comparing diagnostic performance of polysomnography and CRM.43 In a recent update, another six studies were added.44 The diagnostic accuracy was defined as the ability of respiratory polygraphy to modify the probability that a patient had an AHI >15/h by polysomnography. Based on a pre-test probability of 64%, the post-test probability after a negative test result would range from 8% (negative likelihood ratio of 0.05) to 23% (negative likelihood ratio of 0.20). The positive likelihood ratios ranged from 1.8 to 23.8 for all studies, and from 5.7 to 23.8 for the evidence level-I studies. The post-test probability after a positive test result would range from 98% (positive likelihood ratio of 23.8) to 90% (positive likelihood ratio of 5.7). However, no outcome-orientated scientific evidence for polysomnography as the best diagnostic tool to decide which patients will benefit from treatment has been published so far. Thus, it has not been shown that symptom relief, daytime vigilance, quality of life or risk of accidents or cardiovascular disease are superior if the diagnosis is based on polysomnography compared with CRM, and the question remains as to how much polysomnography contributes to treatment decision compared with pure clinical judgement or less expensive tools such as CRM.35,42,45
In a study on outcomes of different nCPAP modes, patients diagnosed by CRM showed treatment effect sizes in respect of respiratory parameters and subjective and objective sleepiness that were comparable to earlier studies with OSAS diagnosed by polysomnography.34,46 In a recent trial, CRM performed as well as polysomnography in the selection of patients who would benefit from nCPAP therapy, challenging polysomnography as the only possible way to diagnose OSA.8 Further research on indications of different diagnostic pathways has been strongly encouraged.43,47 Pulse Oximetry
Pulse oximetry is non-invasive, convenient and widely used in sleep medicine. The technique performs well in tracking fluctuations in arterial oxygen saturation that are characteristic for repetitive breathing disturbance in patients with sleep apnoea. It is regularly integrated into polysomnography and CRM and, by itself, is commonly used in ‘screening’ for sleep apnoea.
In clinical practice, scoring of desaturations and pulse variation is performed by computed analysis on most occasions. When compared with polysomnography, the sensitivity of pulse oximetry ranged from 88 to 98%, and the specificity from 40 to 88% if an AHI of 10/h or 15/h measured was defined as the upper limit of normal.48 Thus, pulse oximetry is not routinely recommended for the diagnosis of OSAS. Most importantly, a ‘negative’ pulsoximetry study should not preclude patients with suspected sleep apnoea from a comprehensive sleep study. However, pulse oximetry may be useful in the monitoring of treatment success in OSAS patients with documented oxygen desaturations prior to initiation of treatment.
Clinical Implications
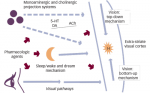
Daytime sleepiness, impaired cognitive performance and quality of life lead patients to seek medical help. OSAS is now well recognised by general practitioners, who will refer their patients to pulmonologists with experience in sleep medicine or specialised sleep laboratories. Tools to non-invasively diagnose OSA are available. A flow diagram to the diagnostic approach is proposed in Figure 1. As an increasing body of evidence points to an association of OSAS and adverse cardiovascular risk, the question remains whether screening could benefit patients with the condition as the evidence supporting the favourable effects of treatment is steadily growing. Recently, screening using nocturnal oximetry for the detection of sleep-related breathing disturbances was recommended for patients with heart failure.54 However, indications to screen for OSA and target subgroups remain to be defined. In a clinical update, experts in the field recommended considering OSA in high-risk patients, especially obese (body mass index >30kg/m2) with refractory hypertension and ‘non-dippers’.55
Figure 1: The Diagnostic Approach to OSAS
Conclusion
As in many other diseases, patient history is still the most important diagnostic tool for the diagnosis of sleep apnoea. Fatigue and a high subjective propensity to fall asleep during the daytime, a history of snoring and breathing pauses during sleep, combined with anthropometric risk factors, make the diagnosis most probable. With a high index of suspicion, simple CRM is appropriate and probably costeffective to confirm the diagnosis. Patients with an equivocal history or inconclusive result after CRM should be offered a full night of polysomnography. In experienced hands, pulse oximetry may be used for screening purposes in well-selected patients; the method also has value in the control of patients under CPAP treatment, providing oxygen desaturations have been documented prior to treatment. In diagnostic uncertainty after equivocal sleep studies, a therapeutic trial should be warranted.