Circadin® (Neurim Pharmaceuticals) is a prolonged-release formulation of 2mg melatonin (PR-melatonin 2mg) that, when taken before bedtime, mimics the physiological pattern of melatonin excretion during the night. It was approved by the European Medicines Agency (EMEA) in June 2007 for the short-term treatment of primary insomnia characterized by poor quality of sleep in patients over 55 years of age. PR-melatonin 2mg is a first-class medicine that goes beyond the facilitation of sleep onset of other widely used drugs for insomnia. This is due to its ability to improve sleep quality, next-day alertness, and quality of life. No significant adverse events were found with PR-melatonin 2mg compared with placebo. It can be used concomitantly with most medications, but potentiates the hypnotic effects of gamma-aminobutyric acid (GABAA) receptor modulators. In contrast to traditional sedative hypnotics, it has shown no evidence of impairing cognitive or psychomotor skills, or of dependence or abuse potential.
Insomnia—Symptoms, Daytime Disturbances, and Treatment Options
Insomnia is the common complaint of difficulty initiating or maintaining sleep and/or experiencing poor quality of sleep (also termed non-restorative sleep, a subjective complaint about tiredness on waking and throughout the day, feeling rested and restored on waking, and the number of awakenings experienced during the night) over at least one month and with negative effects on subsequent daytime functioning.1–3 Patients may suffer immensely from a poor quality of sleep while their sleep quantity is within the normal limits.1,2 Insomnia is a very common disorder, and its prevalence increases with age4–7 and is 1.5 times higher in women than in men.8,9 The disorder may be primary, namely not attributable to any known physical or mental condition or environmental cause, or secondary, resulting from an existing physical or mental condition. The prevalence of poor sleep quality increases with age.10–12 Insomnia also has negative consequences on health-related quality of life.13–17 More so than poor sleep quantity, poor sleep quality corresponds negatively to physical and mental measures of health, wellbeing, activities of daily living, driving skills, memory, productivity, and satisfaction with life.10,11,18–23
The management of insomnia involves non-pharmacological and pharmacological approaches, and traditionally focuses on alleviating difficulties in initiating or maintaining sleep. The most commonly prescribed drugs for insomnia are benzodiazepines (e.g. temazepam) and non-benzodiazepine (e.g. zopiclone, zolpidem) hypnotics, which potentiate the central nervous system (CNS)-suppressant activity of brain GABAA receptors.24 None of these improve subsequent daytime functioning and they are all associated with a higher risk for driving accidents, falls and fractures, overdose, and cognitive impairment, along with the potential for abuse and dependence;25 therefore, their use is discouraged, particularly in elderly patients.26 An unmet medical need remains for a drug that improves quality of sleep. Thus, treatment focus has shifted to re-establishing restorative sleep, improving daytime functioning and quality of life, and avoiding withdrawal symptoms.26–28
Melatonin—A Physiological Sleep Regulator
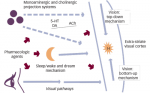
Melatonin (N-acetyl-5-methoxytryptamine) is produced by the pineal gland in a process that is regulated by the internal biological clock, which is localized in the suprachiasmatic nuclei (SCN) of the hypothalamus and inhibited by light perceived by the retina.29 Normally, endogenous melatonin levels rise soon after the onset of darkness, peak in the middle of the night, and gradually decline toward the morning.30 Melatonin serves as a physiological signal of darkness to re-set the biological clock in order to match the environmental day–night cycle and regulate the sleep–wake and other circadian rhythms (e.g. temperature, blood pressure, and hormones).31–33 Melatonin undergoes first-pass hepatic metabolism (half-life in human serum is approximately 40 minutes)34 and over 80% is excreted exclusively in the urine as 6-sulfatoxymelatonin (6-SMT).35 Melatonin is thought to act via its own receptors (MT1, MT2), which are members of the G-protein-linked receptor family.36 The presence of MT1 and MT2 receptors in the SCN, hippocampus, and other brain areas, and melatonin’s physiological activities in these areas, implicates these receptors in the regulation of sleep and circadian rhythms and, perhaps, memory consolidation.37–42
Circadin—A Prolonged-release Melatonin Formulation
The production of melatonin decreases with age.43–45 Lower production of melatonin was found in patients above 55 years of age who suffered from poor sleep quality than in healthy elderly people without such a complaint.44–48 Melatonin therapy may replenish the deficiency in the endogenous sleep-regulating hormones to improve sleep quality and reinforce the functioning of the circadian clock such that the increase in sleep propensity is in tune with the societal activity cycle.49 Due to its short half-life,50 maintaining effective bodily concentrations of melatonin throughout the night requires either repeated administration or a prolonged-release formulation. Circadin is a prolonged-release formulation containing 2mg melatonin (PR-melatonin 2mg), and releases the hormone into the gut over an extended period of time, thereby mimicking physiological patterns of melatonin secretion. Peak plasma concentrations are reached three hours after dosing, with a plateau time of 3.5 hours, before gradually declining to reach baseline levels within 10 hours (see Figure 1).50,51 The drug is primarily metabolized by cytochrome P450 1A2 (CYP1A2) (into the inactive metabolite 6-SMT), and concomitant use of CYP1A2 inhibitors such as fluvoxamine increases its plasma levels.
Clinical Efficacy
Early double-blind, randomized, placebo-controlled studies in insomnia patients over 55 years of age demonstrated the beneficial effects of seven to 21 days of treatment with 2mg per night of Circadin on sleep quantity parameters (latency, wake after sleep onset).52,53 Other randomized, controlled, cross-over studies indicated comparable hypnotic effects of PR-melatonin 2mg to those of the most frequently prescribed hypnotics in aircrew for sleep induction and maintenance.53 In line with the current sleep medicine recommendations, Circadin’s clinical development focused on demonstrating quality of sleep and next-day functioning beyond the facilitation of sleep onset. Given the age-dependent decline in melatonin production, the target population comprised patients suffering from primary insomnia above 55 years of age. In a sleep laboratory trial of PR-melatonin 2mg with a run-in of two weeks (single-blind with placebo treatment), followed by a treatment period of three weeks (double-blind, placebo-controlled, parallel-group design) and a three-week withdrawal, polysomnographically (PSG) assessed sleep latency was shortened by nine minutes compared with placebo.51 There were no modifications of sleep architecture and no effect on rapid eye movement (REM) sleep duration using PR-melatonin 2mg. Significant improvements of diurnal psychomotor skills (measured using critical flicker fusion [CFF] and total reaction time tests) were observed with PR-melatonin 2mg compared with placebo. The PSG recording indicated return of all sleep variables to baseline values one day after ending treatment. No withdrawal or rebound effects were observed in the sleep variables, psychomotor performance, or safety measures.54
Two pivotal clinical studies assessed the effects of PR-melatonin 2mg on sleep quality and subsequent morning alertness.55,56 In a study of 170 outpatients with a two-week run-in with placebo, a randomized, double-blind, placebo-controlled, parallel-group treatment period of three weeks, and a two-week withdrawal with placebo, the rate of patients who showed a clinically significant improvement in both quality of sleep and morning alertness was 47% with PR-melatonin 2mg compared with 27% with placebo (p=0.009). In addition, quality of sleep and morning alertness significantly improved with PR-melatonin 2mg compared with placebo. The complete response was developed within six days and maintained throughout the three-week treatment period. During the two-week withdrawal period, sleep variables gradually returned to baseline, with no rebound and no increase in adverse events or withdrawal symptoms.55
In a second study of 354 outpatients with a two-week run-in with placebo and a randomized, double-blind, placebo-controlled, parallel-group treatment period of three weeks, the percentage of patients who showed a clinically significant improvement in both quality of sleep and morning alertness was 26% with PR-melatonin 2mg compared with 15% with placebo (p=0.014). A significant and clinically relevant shortening of sleep latency, similar to most frequently used sleep medications, was also found (-24.3 versus -12.9 minutes; p=0.028), and was consistent with that previously found in the sleep laboratory trial.51,56 In addition, self-reported quality of sleep, number of awakenings, and morning alertness of patients significantly improved with PR-melatonin 2mg compared with placebo. Quality of life improved significantly with PR-melatonin 2mg compared with placebo (p=0.034). The incidence of adverse events was low and most side effects were judged to be of minor severity.56 A pooled analysis indicated that clinical response—defined as a ‘substantial improvement’ for both quality of sleep and morning alertness— was 32.4% with PR-melatonin 2mg versus 18.7% with placebo (p=0.0003). The percentage of patients with a clinically relevant improvement in quality of sleep or morning alertness was 48 versus 34.5% (p=0.0017) and 40.3 versus 30% (p=0.012), respectively.51
Clinical Safety
Pre-clinical data on melatonin have not revealed any effects to prompt concern over its long-term use in humans at the clinical dose of PR-melatonin 2mg. Unlike commonly prescribed hypnotic drugs, PR-melatonin 2mg has no deleterious effect on psychomotor performance after single57 or repeated doses.51 The total exposure of patients to PR-melatonin 2mg comprised 1,926 patients in short-term studies, 373 patients who received the compound for six months, and 146 patients who received PR-melatonin for one year or longer.54 No safety concerns were raised. The most common adverse events (>2%) were headache, pharyngitis, back pain, and asthenias, and were probably not related to treatment. When normalized for exposure period (100 patient-weeks), there were fewer adverse events with PR-melatonin 2mg than with placebo (3.17 versus 8.21, respectively). PR-melatonin 2mg potentiates the hypnotic effects of benzodiazepines,58,59 and use of such combinations should thus be well controlled. Discontinuation of PR-melatonin 2mg after 21 nights did not produce rebound or withdrawal phenomena.54,55
A dose-ranging study in 257 insomnia outpatients aged between 20 and 80 years with a two-week run-in (placebo), six weeks of treatment (randomized, double-blind, placebo-controlled, parallel-group), six to 12 months of PR-melatonin 2mg (single-blind), and a two-week withdrawal period demonstrated an optimal dose of 2mg with a significantly greater benefit in patients above 55 years of age (Lemoine P, Zisapel N, et al., unpublished data). The mean week-by-week percentage of nights scored as ‘good’ or ‘very good’ (diary records) increased during the PR-melatonin 2mg treatment to reach a plateau level that was maintained throughout the six to 12 months of treatment and slowly declined during the two-week withdrawal period, thus suggesting a remnant effect after discontinuation. No rebound or withdrawal phenomena were observed, even after a prolonged period (12 months) of treatment with PR-melatonin 2mg (see Figure 2; Lemoine P, Zisapel N, et al., unpublished data).
Melatonin Dietary Supplements
Circadin is a medicinal drug developed according to US Food and Drug Administration (FDA) and EU drug legislation, and has to be prescribed by a doctor within a specific indication. This is a guarantee of quality, efficacy, and safety for the patient. Heavy media attention, including CNN, CBS, and major newspaper coverage, was focused on melatonin in 1994 and 1995, overstating the effects of this compound even though these health claims have never been evaluated for efficacy and safety in large-scale clinical trials compliant with regulatory requirements. With the passage of the ‘Dietary Supplement Health and Education Act’ in 1994, melatonin became widely available in the US under variable dosage forms of unknown purity and questionable quality. In addition, as no standardization is required, the active ingredient may be absent or highly variable among manufacturers.60 Some batches of melatonin have been found to contain contaminants and impurities that can be harmful for the patient, mostly due to the lack of requirements for good manufacturing practices.61–64 The presence of such impurities in commercially available melatonin raises serious questions about possible consequences after long-term consumption, especially when used at higher than recommended doses.65 In addition, melatonin food supplements in fast-release formulations provide a peak of melatonin at the beginning of the night, which quickly wears off. They do not allow for sustained efficacy throughout the night and may even result in phase shifting of the endogenous biological clock.66,67 The so-called controlled-release formulations of the dietary supplements are not well defined and their benefit has not been demonstrated. Furthermore, not all of the risks, side effects, or interactions associated with the use of such products are known because they have not been tested in controlled large-scale clinical trials compliant with regulatory requirements.64
Conclusions
Although many of the outcomes of insomnia derive from the extent to which it impairs daytime functioning, insomnia drugs were developed for sleep induction but not poor sleep quality and next-day performance. Circadin, designed to generate a profile more closely related to the endogenous release profile of melatonin, improves sleep quality and facilitates sleep onset in insomnia patients above 55 years of age and improves morning alertness and quality of life. The significantly higher responder rate in the PR-melatonin 2mg group compared with the placebo group establishes the clinical relevance of the observed effects. The efficacy of PR-melatonin 2mg in insomnia patients >55 years of age derives from its physiological functions as a sleep regulator and circadian clock synchronizer. A clinical response defined as a ‘concomitant and clinically substantial improvement’ on two variables assessing the quality of sleep and the impact on diurnal behavior is seen in 32% of patients. Nevertheless, it is noted that the percentage of patients improving on one of the sleep quality variables is considerably higher (48%). In addition to these effects, PR-melatonin 2mg improves sleep onset latency, similar to other insomnia drugs. A limitation is that full efficacy develops over a number of days and therefore cannot be demonstrated after a single dose of the drug. Furthermore, although insomnia tends to be chronic, the drug is currently indicated in the EU only for short-term periods (three weeks), although long-term safety trials have been performed and indicated that there are no safety issues of long-term use and subsequent discontinuation.51 In particular, PR-melatonin 2mg treatment is not associated with cognitive impairments or residual daytime (‘hangover’) effects, and patients suffer no rebound insomnia or withdrawal symptoms upon discontinuation. Therefore, Circadin might provide us with a new and useful therapeutic principle in insomnia therapy among older adults. ■