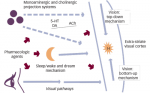
Treatment Options
Behavioral changes, specifically weight loss, a reduction in alcohol consumption, and the cessation of cigarette smoking, can all significantly reduce the symptoms of OSA, and represent an important foundation of treatment. These recommendations are generally appropriate for all patients with OSA, but may be of significant value to those with mild OSA, as they may preclude more aggressive treatment approaches. However, in most cases recommendations for behavioral modifications are combined with nasal continuous positive airway pressure (nCPAP), which is considered to be the first-line therapy for moderate to severe OSA. The efficacy of nCPAP is well established, but compliance can be problematic for some patients. More recently, oral appliances that improve the patency of the upper airway by reinforcing its stability have become treatment options. Finally, surgical interventions for OSA, including uvulopalatopharyngoplasty (UPPP), laser-assisted uvulopalatopharyngoplast (LAUP), maxillo-mandibular advancement, and bariatric surgery, may all be considered, but tend to be most appropriate for patients who are unable or unwilling to comply with medical management of the condition.
Drug treatments for OSA have been considered and are currently in development. For example, BGC20–0166, a proprietary combination of two marketed serotonergic modulating drugs, is being tested in OSA patients to determine its efficacy in reducing the apnea–hypopnea index (AHI).8 The mechanism of this effect is believed to be related to increases in upper airway muscle tone and respiratory drive. Studies of BGC20–0166 in a rat model of sleep apnea indicate that it reduces the AHI by 90%. More recently, a 28-day double-blind, parallel-group, placebocontrolled polysomnographic study of BGC20–0166 in patients with sleep apnea revealed that it resulted in a 40% reduction in the mean AHI, relative to placebo, after 28 days of treatment. Oximetry revealed a trend in oxygen saturation that was consistent with the reduction in AHI, with no notable differences in the number of subjects with adverse events in the placebo and active drug treatment groups. These findings suggest that promising new therapeutics for sleep apnea are in development. However, as yet there is no drug treatment specifically indicated for OSA.
Unfortunately, despite the best efforts of the practitioner and patient, even with adequate use of nCPAP daytime sleepiness can persist.9–12 Modafinil, a wakefulness-promoting agent, was one of the first compounds to be evaluated for its ability to improve wakefulness in patients with excessive sleepiness associated with several sleep disorders, including OSA.10,13,14 According to a recent search of the National Institutes of Health (NIH) website, a small number of trials of other drugs have been conducted in recent years. One trial compared modafinil with xyrem and zolpidem, another evaluated pantoprazole in patients with OSA and comorbid acid reflux, and two others evaluated mometasone furoate nasal spray in patients with OSA associated with perennial allergic rhinitis. Armodafinil
In recent years, armodafinil, an isomer of modafinil, has become the most promising new therapy for excessive sleepiness associated with OSA. It was approved by the US Food and Drug Administration (FDA) in 2007 to improve wakefulness in patients with excessive sleepiness associated with OSA, narcolepsy, or shift-work sleep disorder. Modafinil is a racemic compound containing an equal amount of the R- and S-enantiomer.15 Rmodafinil has a significantly longer half-life (10–14 versus three to four hours)16–18 and is eliminated three times more slowly than S-modafinil.17 The differences seen in the metabolism of these compounds can result in significant differences in the plasma concentrations of the two enantiomers. Unsurprisingly, dosing with armodafinil (R-modafinil) has been shown to produce higher plasma concentrations later in the day than modafinil on a milligram-to-milligram basis and produces greater improvements in wakefulness and attention span in healthy subjects.15
The approval of armodafinil for use in OSA patients was based on the results of two 12-week trials in this population.19,20 Both studies enrolled patients who were regular and adequate users of nCPAP but who still experienced residual excessive sleepiness. The design of both studies was similar: both performed assessments at baseline and weeks four, eight, and 12. Assessments included the Maintenance of Wakefulness Test (MWT), a Clinical Global Impression of Change (CGI-C) scale, the Epworth Sleepiness Scale (ESS), the Brief Fatigue Inventory (BFI), and the Cognitive Drug Research (CDR) battery. The MWT and CDR batteries were performed repeatedly during each assessment visit. The MWT commenced at 09:00, 11:00, 13:00, 15:00, 17:00, and 19:00 hours, followed by the CDR battery at 09:30, 11:30, 15:30, 17:30, and 19:30 hours. Results from the MWT were averaged across the first four and the last three assessments to evaluate differences in alertness in both the morning and afternoon. CDR results were averaged in a similar manner.
The first study compared armodafinil 150mg with placebo in 259 subjects.19 Armodafinil significantly improved wakefulness compared with placebo (as measured by morning MWT assessments at four, eight, and 12 weeks; p<0.01). Only afternoon MWT assessments differed significantly from placebo at week 12. Episodic secondary memory (measured by the CDR battery) was significantly improved compared with placebo during the morning assessment at week 12 only. At each visit, the CGI-C indicated that armodafinil significantly improved the subject’s overall clinical condition compared with placebo (p<0.05). Similarly, the ESS was significantly improved relative to changes in the placebo group for subjects randomized to active treatment at all time-points (p<0.01), and the BFI showed a significant improvement in overall fatigue with armodafinil at weeks four and 12. The second study evaluated the efficacy of 150 and 250mg of armodafinil relative to placebo in a total of 392 subjects.20 MWT assessments indicated that armodafinil 250mg significantly improved morning wakefulness at weeks four, eight, and 12, while the 150mg dose group saw significant improvement at weeks four and 12 (p<0.05). Afternoon MWT assessments found that both doses of armodafinil were indistinguishable from placebo. The CDR battery recorded significant improvements in morning episodic secondary memory with both doses at week four (p<0.05) and at week eight with the 250mg dose group only (p<0.01). Other measures and time-points did not reach the level of significance. A significantly greater number of subjects were rated as at least minimally improved on the CGI-C in both armodafinil dose groups relative to placebo at all visits (p<0.001). As seen in the first study, significantly greater improvements in the ESS were seen with both doses of armodafinil at all time-points (p<0.001) than with placebo. Global fatigue scores on the BFI were significantly improved (p<0.05) with active treatment relative to placebo at weeks four (150mg only), eight (250mg only), and 12 (both dose groups). Armodafinil was generally safe and well tolerated in both studies. A pooled analysis of adverse events across the two 12-week studies (armodafinil n=391, placebo n=260) found that the most common adverse events were headache (17% armodafinil versus 8% placebo), nausea (6 versus 4%), insomnia (6 versus 1%), dizziness (5 versus 2%), and anxiety (5 versus <1%).21 No clinically meaningful changes relative to baseline values were observed in clinical laboratory assessments, vital signs, electrocardiogram parameters, or physical examinations.
The duration of nCPAP therapy was assessed at baseline and the final visit to evaluate armodafinil’s impact on nCPAP compliance. In both studies nCPAP use was approximately seven hours after baseline. Values remained high for both active and placebo treatment groups throughout the study period. However, a small decline in use was observed in both treatment groups. nCPAP usage declined by -0.3 (0.7 standard deviation) hours in armodafinil subjects and by -0.1 (0.6) hours in placebo-treated subjects. This was a between-group difference of approximately 12 minutes (p<0.0001). At the final visits, AHI values were low and comparable between treatment groups, and no significant changes were observed relative to baseline polysomnography-measured sleep variables.
Conclusion
Excessive sleepiness is a debilitating condition associated with OSA that has a profound effect on patients, their families, co-workers, and the public at large.22–24 Excessive sleepiness can negatively influence cognition and impair both occupational and social functioning.24–27 Even when OSA is appropriately controlled by nCPAP, excessive sleepiness can persist and continue to influence a patient’s quality of life. Several compounds, including modafinil, xyrem, zolpidem, pantoprazole, and mometasone furoate nasal spray, have been evaluated for the tretament of excessive sleepiness. However, armodafinil appears to be the most recent promising therapy for this condition. Armodafinil has been approved to improve wakefulness in patients with excessive sleepiness associated with OSA based on the results of two trials in OSA patients compliant with nCPAP therapy. In both studies, armodafinil safely improved wakefulness and reduced fatigue compared with placebo over the course of 12 weeks of treatment.