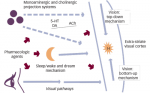
Kynurenine is further metabolized along two distinct routes:
- the kynurenine–kynurenic acid (KYNA) pathway, regulated by kynurenine amino transferase (in both astrocytes and microglia) and resulting in production of KYNA, the only known endogenous N-methyl-D-aspartic acid (NMDA) antagonist; and
- the kynurenine–(quinolinic acid)–nicotinic acid pathway, which is initiated by kynurenine hydroxylase in microglia, but not in astrocytes, and results in the production of NMDA agonists and free radical generators (e.g. quinolinic and picolinic acids), the precursors of nicotinic acid.
The crosstalk between the methoxyindole and kynurenine pathways is provided by NMDA-agonist-induced stimulation and NMDA-antagonist- induced inhibition of melatonin formation from serotonin, respectively. A type 1 immune response triggers microglial production of cytokines able to induce IDO. The most powerful inducer of IDO is interferon (IFN)-g. The other type-1 cytokine, tumor necrosis factor (TNF)-α, stimulates and/or drastically potentiates IFN-γ-induced IDO activity. Production of IFN-γand TNF-αis controlled by (IFN-γ)+874 (T/A) and (TNF-α)-308 (G/A) genotypes, respectively. The high promoter T allele is associated with high IFN-γ production and increased IDO activity (i.e. elevated plasma kynurenine levels and kynurenine/tryptophan ratios) in healthy individuals. The presence of (TNF-α)-308 high promoter (A) may, therefore, strengthen the association between (IFN-γ)+874 high promoter (T) and IDO activity.
There are no published studies of IFN-γ gene polymorphism in schizophrenia. The TNF-αA allele is associated with high vulnerability to the late-onset paranoid-type schizophrenia in males. Genetic regulation of IDO may be affected by hormones; although IDO is not inducible by hormones, application of hydrocortisone, dexamethasone, and prolactin drastically potentiates IFN-γ-induced IDO, while the expression of the IFN-γ gene may be subject to direct hormonal control by estradiol and prolactin.
The type 2 immune response—which is predominant in schizophrenia—is characterized by inhibition of IDO in microglia and activation of TDO in astrocytes. Due to the the absence of kynurenine hydroxylase in astrocytes, activation of TDO results in a shift from the kynurenine–(quinolinic acid)–nicotinic acid to the kynurenine–KYNA athway. Increased levels of KYNA in the brain (particularly in the pre- frontal cortex) and cerebrospinal fluid (CSF) in schizophrenia may be accounted for by dopaminergic hyperfunction/glutaminergic hypofunction (and related clinical manifestations) in schizophrenia, as KYNA—the only known endogenous NMDA antagonist—activates mid-brain dopaminergic neurons similar to the effect of MK-801, an exogenous NMDA antagonist and psychotomimetic. Furthermore, the higher affinity of KYNA antagonism to a-7-nicotinic acetylcholine receptors than to NMDA receptors may explain the existence of cognitive impairment without psychotic symptoms, while psychotic symptoms are always associated with cognitive impairment.
Cognitive impairment in schizophrenia may also be mediated by the metabolites of the kynurenine–nicotinic acid pathway, such as quinolinic and picolinic acid (NMDA agonists), and 3-hydroxykynurenine and 3-hydroxyanthranilic acids (free-radical generators). Quinolinic and picolinic acids activate inducible nitric oxide synthase (iNOS). NO derived from the iNOS pathway is a free radical that, by reacting with superoxide, forms an even more potent oxidant: peroxynitrite. NO derived from the iNOS pathway mediates cellular toxicity and triggers a cPLA2–lipid peroxidation cascade, which contributes to myelin degradation.
The availability of TRY as a substrate is one of the rate-limiting factors of serotonin biosynthesis. The shift of TRY metabolism from the TRY–serotonin to the TRY–kynurenine pathway may be responsible for symptoms of depression observed in schizophrenia. The decreased availability of TRY as a substrate to serotonin biosynthesis may be further accentuated by kynurenine-induced inhibition of TRY transport via the blood–brain barrier. The decreased formation of serotonin as a substrate of melatonin biosynthesis as a result of the shift from the TRY–serotonin to the TRY–kynurenine pathway may negatively affect melatonin formation. The shift from the kynurenine–nicotinic acid to the kynurenine–KYNA pathway may further impair melatonin biosynthesis, since KYNA may— in a similar way to the exogenous NMDA antagonist MK-801—inhibit the rate-limiting step of melatonin biosynthesis: serotonin N-acetylation. The lack of night- time melatonin production was indeed described in patients suffering from schizophrenia; this deficiency may contribute to the sleep and other circadian rhythm disturbances observed in schizophrenia. A review of data from the recent literature suggests that genetically controlled immune system responses to peri-natal environmental challenges (e.g. infection, ischemia) may result in TRY metabolism changes that are important for the pathogenesis of schizophrenia. These changes are a shift from the TRY–serotonin–melatonin to the TRY–kynurenine pathway, and from the kynurenine–nicotinic acid to the kynurenine–KYNA pathway. Considering the prominent role of KYNA in the pathogenesis of schizophrenia, the obvious therapeutic target is the suppression of KYNA production. It is noteworthy that chronic administration of antipsychotics decreased levels of KYNA in rat brains. Suppression of KYNA production by selective cyclo-oxygenase (COX-2) inhibitors was successful in some— though not all—trials; COX-1 inhibitors, on the other hand, stimulate KYNA production. It has been suggested that anti-inflammatory therapy is more effective during the first years of the disease.
Inhibition of TDO may be another target for therapeutic intervention. Melatonin has been shown to have a strong suppressive effect on liver TDO. Considering the availability of melatonin (as a food supplement) and its virtual lack of toxicity, the clinical trials may be of interest. It is noteworthy that pineal gland extracts were reported to produce benefits in patients with schizophrenia in the uncontrolled clinical trials conducted at McLean Hospital (Boston, MA) in the early 1950s. The use of melatonin and its immediate precursor, N-acetylserotonin, may be advantageous due to the inhibitory effect of these agents on cytokine production and iNOS. The comprehensive studies of gene polymorphism in relation to levels of TRY, kynurenine, and KYNA may allow the early identification of individuals at risk for schizophrenia.